Measure Information Form
Version 2018A
Measure Information Form
| Set Measure ID | Performance Measure Name |
|---|---|
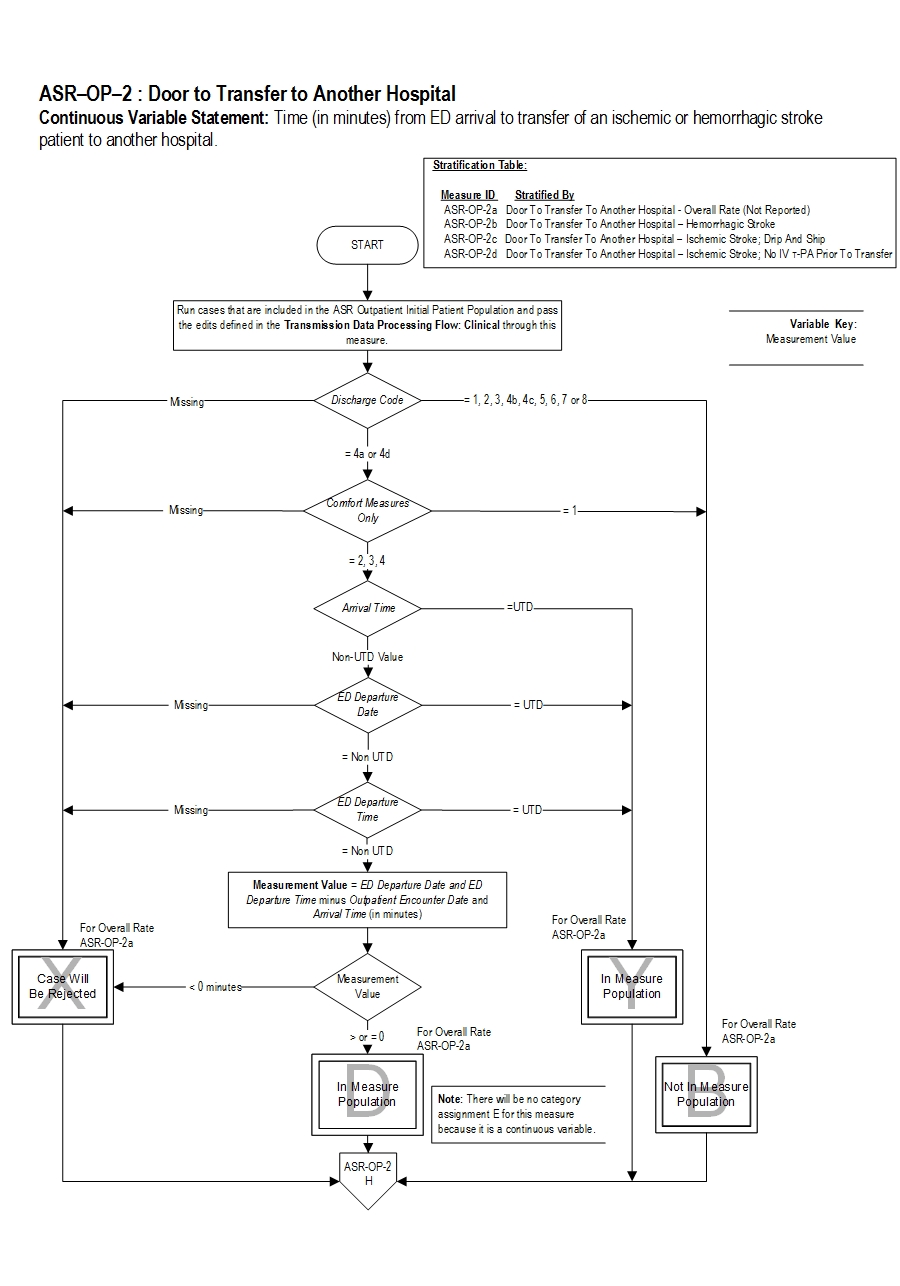
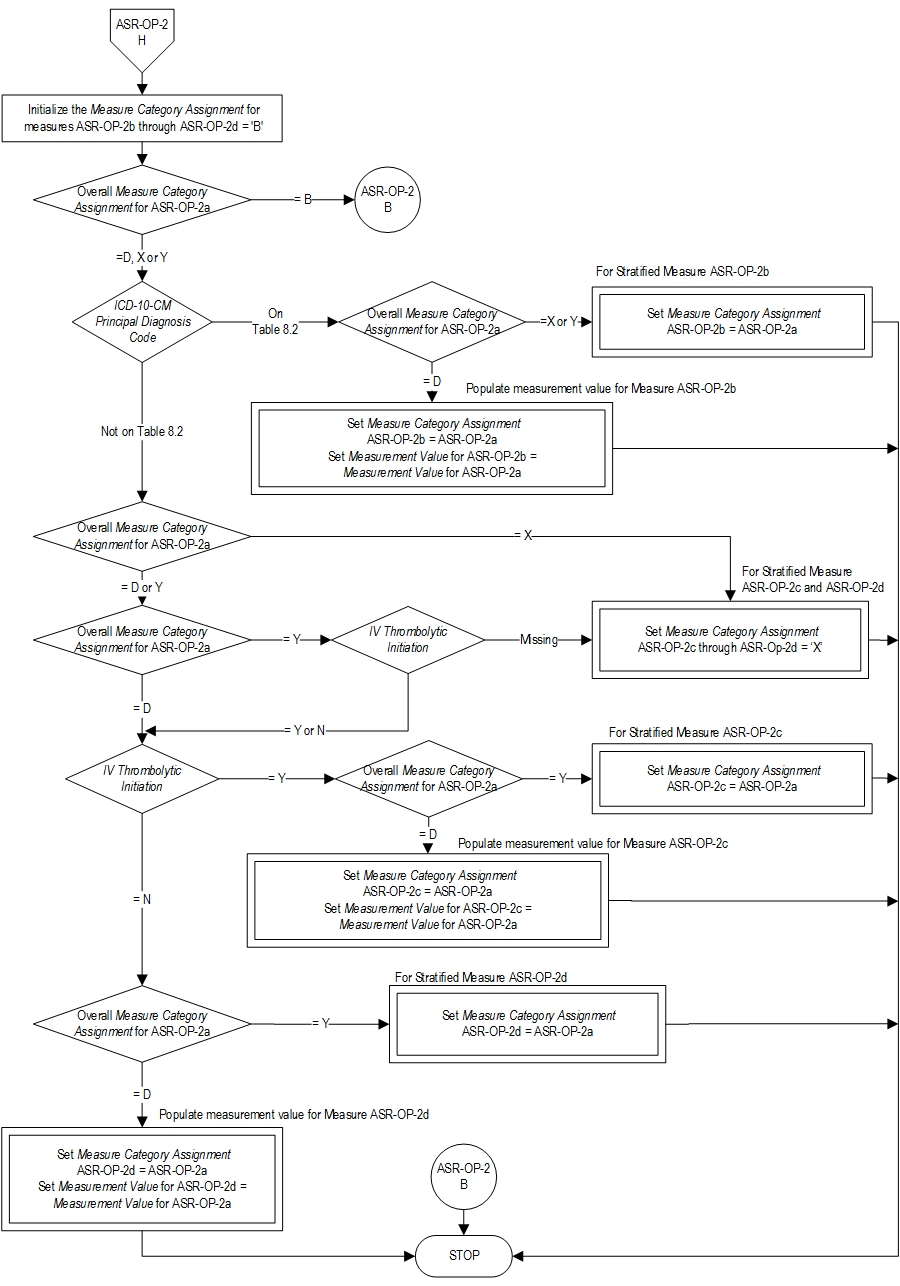
| ASR-OP-2a | Door to Transfer to Another Hospital - Overall Rate |
| ASR-OP-2b | Door to Transfer to Another Hospital - Hemorrhagic Stroke |
| ASR-OP-2c | Door to Transfer to Another Hospital - Ischemic Stroke; Drip and Ship |
| ASR-OP-2d | Door to Transfer to Another Hospital - Ischemic Stroke; No IV t-PA Prior to Transfer |
Most patients with an acute stroke seen initially at an ASRH will require emergent transfer to a PSC or CSC. The Brain Attack Coalition recommends that such transfers occur within 2 hours of the patient presenting to the ASRH (Alberts, 2013). Additionally, written transfer agreements between the ASRH and at least one PSC or CSC and a transportation vendor with both ground and air ambulance transfer options are recommended. One in four patients are transferred while receiving intravenous (IV) thrombolytic therapy (t-PA) (Sheth, 2015); others transferred after initiation of coagulopathy reversal treatment. Reducing the time stroke patients remain in the emergency department (ED) can improve access to a higher-level of stroke care and advanced intra-arterial or endovascular treatments, and increase quality of care. For those stroke patients who are not transferred to a PSC or CSC, inpatient admission within 3 hours, preferably to a formal stroke unit, is recommended (Jauch, 2013).
Type of Measure: Process Improvement Noted As: Decrease in the median valueASR-2b Time (in minutes) from ED arrival to transfer of a hemorrhagic stroke patient to another hospital
ASR-2c Time (in minutes) from ED arrival to transfer of an ischemic stroke patient (drip and ship) to another hospital
ASR-2d Time (in minutes) from ED arrival to transfer of an ischemic stroke patient (no IV t-PA prior to transfer) to another hospital
Included Populations:AND
- Patients with an ICD-10-CM Principal Diagnosis Code for ischemic or hemorrhagic stroke as defined in Appendix A, Table 8.1 or Table 8.2
AND
- Patients who are transferred to another hospital
Excluded Populations:
- An E/M Code for emergency department encounter as defined in Appendix A, Table 1.0
Data Elements:
- Patients less than 18 years of age
- Patients with Comfort Measures Only documented on day of or day after arrival
- Patients who expired in the emergency department
- Discharges to dispositions other than an acute care facility
- Alberts MJ, Wechsler LR, Jensen MEL, Lachtaw RE, Crocco TJ, George MG, Baranski J, Bass RR, et al. “Formation and Function of Acute Stroke-Ready Hospitals Within a Stroke System of Care Recommendations From the Brain Attack Coalition” [In Eng]. Stroke (Nov 12 2013).
- Albright KC, Branas CC, Meyer BC, Matherne-Meyer DE, Zivin JA, Lyden PD, Carr BG. “Acute Cerebrovascular Care in Emergency Stroke Systems.” [In Eng]. Arch Neurol (Oct 2010).
- American Heart Association. Acute Stroke Ready Hospital, 2015.
- Jauch, E. C., J. L. Saver, H. P. Adams, Jr., A. Bruno, J. J. Connors, B. M. Demaerschalk, P. Khatri, et al. "Guidelines for the Early Management of Patients with Acute Ischemic Stroke: A Guideline for Healthcare Professionals from the American Heart Association/American Stroke Association." [In Eng]. Stroke (Jan 31 2013).
- Lyerly MJ, Albright KC, Boehme AK, Shahripour RB, Donnelly JP, Houston JT, Rawal PV, Kapoor N, Alvi M, Sisson A, Alexandrov AW, Alexandrov AV. “Patient Selection for Drip and Ship Thrombolysis in Acute Ischemic Stroke”. [In Eng]. South Med J (Jul 2015).
- Sheth KN, Smith EE, Grau-Sepulveda MV, Kleindorfer D, Fonarow GC, Schwamm LH. "Drip and Ship Thrombolytic Therapy for Acute Ischemic Stroke: Use, Temporal Trends, and Outcomes.” [In Eng]. Stoke (Mar 2015).