Release Notes:
Measure Information Form
Version 2015A1
**NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE**Measure Information Form
Measure Set: Perinatal Care(PC)
Set Measure ID: PC-02
Performance Measure Name: Cesarean Section
Description: Nulliparous women with a term, singleton baby in a vertex position delivered by cesarean section
Rationale: The removal of any pressure to not perform a cesarean birth has led to a skyrocketing of hospital, state and national cesarean section (CS) rates. Some hospitals now have CS rates over 50%. Hospitals with CS rates at 15-20% have infant outcomes that are just as good and better maternal outcomes (Gould et al., 2004). There are no data that higher rates improve any outcomes, yet the CS rates continue to rise. This measure seeks to focus attention on the most variable portion of the CS epidemic, the term labor CS in nulliparous women. This population segment accounts for the large majority of the variable portion of the CS rate, and is the area most affected by subjectivity.
As compared to other CS measures, what is different about NTSV CS rate (Low-risk Primary CS in first births) is that there are clear cut quality improvement activities that can be done to address the differences. Main et al. (2006) found that over 60% of the variation among hospitals can be attributed to first birth labor induction rates and first birth early labor admission rates. The results showed if labor was forced when the cervix was not ready the outcomes were poorer. Alfirevic et al. (2004) also showed that labor and delivery guidelines can make a difference in labor outcomes. Many authors have shown that physician factors, rather than patient characteristics or obstetric diagnoses are the major driver for the difference in rates within a hospital (Berkowitz, et al., 1989; Goyert et al., 1989; Luthy et al., 2003). The dramatic variation in NTSV rates seen in all populations studied is striking according to Menacker (2006). Hospitals within a state (Coonrod et al., 2008; California Office of Statewide Hospital Planning and Development [OSHPD], 2007) and physicians within a hospital (Main, 1999) have rates with a 3-5 fold variation.
Type of Measure: Outcome
Improvement Noted As: Decrease in the rate
Numerator Statement: Patients with cesarean sections
Included Populations:
ICD-9-CM Principal Procedure Code or ICD-9-CM Other Procedure Codes for cesarean section as defined in Appendix A, Table 11.06
Excluded Populations: None
Data Elements:
Denominator Statement: Nulliparous patients delivered of a live term singleton newborn in vertex presentation
Included Populations:
- ICD-9-CM Principal or ICD-9-CM Other Diagnosis Codes for pregnancy as defined in Appendix A, Table 11.01, 11.02, 11.03 or 11.04
- Nulliparous patients with ICD-9-CM Principal Diagnosis Code or ICD-9-CM Other Diagnosis Codes for outcome of delivery as defined in Appendix A, Table 11.08 and with a delivery of a newborn with 37 weeks or more of gestation completed
Excluded Populations:
- ICD-9-CM Principal Diagnosis Code or ICD-9-CM Other Diagnosis Codes for multiple gestations and other presentations as defined in Appendix A, Table 11.09
- Less than 8 years of age
- Greater than or equal to 65 years of age
- Length of Stay >120 days
- Enrolled in clinical trials
- Gestational Age < 37 weeks or UTD
Data Elements:
Continuous Variable Statement:
Included Populations:
Excluded Populations:
Data Elements:
- [[Manual.TableOfContents][]]
- [[Manual.SamplingHCSS][]]
- [[Manual.ReleaseRecord0014PublishRecord][]]
- [[Manual.ReleaseRecord0017PublishRecord][]]
- [[Manual.ReleaseNotes][]]
- [[Manual.DataCluster004Form][]]
- [[Manual.TypeOfMeasure05][]]
- [[Manual.UseStatus02][]]
- [[Manual.DataCluster009][]]
- [[Manual.TransmissionChapter][]]
- [[Manual.QuestionCategoryID17][]]
- [[Manual.AppendixACTSK][]]
- [[Manual.SCR00000][]]
- [[Manual.MeasureSetEditTemplate][]]
- [[Manual.ReleaseRecord0001][]]
- [[Manual.ReleaseRecord0032PublishForm][]]
- [[Manual.QuestionCategoryID03][]]
- [[Manual.AppendixPTJC][]]
- [[Manual.QuestionCategoryID47][]]
- [[Manual.MeasureQuestionSearch][]]
- [[Manual.QuestionCategoryID38][]]
- [[Manual.RenderSpecificationChangeRequest][]]
- [[Manual.MissingDataChapter][]]
- [[Manual.SpecificationChangeRequestTemplate][]]
- [[Manual.AppendixDTJC][]]
- [[Manual.AppendixBTJC][]]
- [[Manual.ImpNoteAsValueID05][]]
- [[Manual.InternetExplorerIssues][]]
- [[Manual.ReleaseRecord0025PublishRecord][]]
- [[Manual.QuestionCategoryID62][]]
- [[Manual.TopicType][]]
- [[Manual.QuestionCategoryID03a][]]
- [[Manual.AdoptionStatus01][]]
- [[Manual.ReleaseRecord0019PublishRecord][]]
- [[Manual.QuestionCategoryID49][]]
- [[Manual.QuestionCategoryID21][]]
- [[Manual.DataCluster015][]]
- [[Manual.GlossaryStroke][]]
- [[Manual.ClassifiedTopic][]]
- [[Manual.DataCluster011Form][]]
- [[Manual.HelpDocuments][]]
- [[Manual.ReleaseRecord0005PublishRecord][]]
- [[Manual.DraValueID01][]]
- [[Manual.WebAtom][]]
- [[Manual.QuestionCategoryID24][]]
- [[Manual.WebAliases][]]
- [[Manual.DataCluster013][]]
- [[Manual.UsingTheManualPBM][]]
- [[Manual.AdminTools][]]
- [[Manual.TableOfContentsPBM][]]
- [[Manual.TestAppendixA][]]
- [[Manual.DataCluster017][]]
- [[Manual.ReleaseRecord0023PublishRecord][]]
- [[Manual.AnotherTest][]]
- [[Manual.AppendixA][]]
- [[Manual.AppendixCTJC][]]
- [[Manual.AppendixH][]]
- [[Manual.CoverPagePBM][]]
- [[Manual.TransmissionAlphaDataDictionaryTJC][]]
- [[Manual.QuestionCategoryID15][]]
- [[Manual.QuestionCategoryID56][]]
- [[Manual.QuestionCategoryID58][]]
- [[Manual.DataUtilizationStroke][]]
- [[Manual.Introduction][]]
- [[Manual.UsingTheManual][]]
- [[Manual.DevStatus00][]]
- [[Manual.DataCluster013Form][]]
- [[Manual.QuestionCategoryID43][]]
- [[Manual.QuestionCategoryID13][]]
- [[Manual.DataCluster006][]]
- [[Manual.HealthcareFrameworkHCSS][]]
- [[Manual.CreateNewTopic][]]
- [[Manual.ImpNoteAsValueID03][]]
- [[Manual.QuestionCategoryID36][]]
- [[Manual.QuestionCategoryID26][]]
- [[Manual.DevStatus01][]]
- [[Manual.OldWebSideBar][]]
- [[Manual.CommentID10002][]]
- [[Manual.QuestionCategoryID05][]]
- [[Manual.WebSearchAdvanced][]]
- [[Manual.FormAttributeValueTemplate][]]
- [[Manual.QuestionCategoryID60][]]
- [[Manual.SCRDetailsID100004][]]
- [[Manual.DataCluster017Form][]]
- [[Manual.QuestionCategoryID53][]]
- [[Manual.Releases][]]
- [[Manual.DataUtilizationHCSS][]]
- [[Manual.ReleaseRecord0024PublishRecord][]]
- [[Manual.DataElement][]]
- [[Manual.DataCollectionApproach][]]
- [[Manual.BCCPopulationAndSampling][]]
- [[Manual.DataCluster006Form][]]
- [[Manual.QuestionCategoryID28][]]
- [[Manual.AppendixDPBM][]]
- [[Manual.QuestionCategoryID25][]]
- [[Manual.DataReportingToolStroke][]]
- [[Manual.ReleaseRecord0033PublishForm][]]
- [[Manual.DataCluster019][]]
- [[Manual.DataCluster018Form][]]
- [[Manual.DataElem0346][]]
- [[Manual.AppendixCPBM][]]
- [[Manual.AppendixAAMICodeTables][]]
- [[Manual.QuestionCategoryID34][]]
- [[Manual.Test2AppendixA][]]
- [[Manual.AppendixATableForm][]]
- [[Manual.PopulationOptionsID01][]]
- [[Manual.QuestionCategoryID52][]]
- [[Manual.PreOpAntibioticProphylaxis][]]
- [[Manual.DiagnosticImagingPET][]]
- [[Manual.MeasureInformationForm][]]
- [[Manual.DataCluster003][]]
- [[Manual.QuestionCategoryID01][]]
- [[Manual.ReleaseRecord0016PublishRecord][]]
- [[Manual.AppendixCCAH][]]
- [[Manual.TableofContentsHCSS][]]
- [[Manual.TransmissionPopulationDataProcessingFlowTJC][]]
- [[Manual.DataCluster004][]]
- [[Manual.DataCluster][]]
- [[Manual.WebChanges][]]
- [[Manual.AppendixAPBM][]]
- [[Manual.DataReportedAs][]]
- [[Manual.StrokeGuidelines][]]
- [[Manual.TopicForm][]]
- [[Manual.IntroductionTJC][]]
- [[Manual.QuestionCategoryID41][]]
- [[Manual.QuestionCategoryID57][]]
- [[Manual.QuestionCategoryID45][]]
- [[Manual.WebCreateNewTopic][]]
- [[Manual.DataCluster002Form][]]
- [[Manual.VTEProphylaxisOptionsforSurgery][]]
- [[Manual.AlphaDataElementList][]]
- [[Manual.AppendixE][]]
- [[Manual.QuestionCategoryID11][]]
- [[Manual.TransmissionDataProcessingFlow][]]
- [[Manual.WebPreferences][]]
- [[Manual.QuestionCategoryID08][]]
- [[Manual.SpecificationChangeRequestForm][]]
- [[Manual.SCRDetailsID100002][]]
- [[Manual.AppendixETJC][]]
- [[Manual.QuestionCategoryID18][]]
- [[Manual.DataCollectionToolsHCSS][]]
- [[Manual.AppendixBPBM][]]
- [[Manual.WebLinksOld][]]
- [[Manual.TypeOfMeasure03][]]
- [[Manual.TransmissionAlphaDataDictionary][]]
- [[Manual.PublishPluginHistory][]]
- [[Manual.QuestionCategoryID32][]]
- [[Manual.AlgorithmOne][]]
- [[Manual.AppendixGTJC][]]
- [[Manual.UseStatus][]]
- [[Manual.DataCollectionApproachID02][]]
- [[Manual.AppendixPTJCcrosswalks][]]
- [[Manual.TableOfContentsTJC][]]
- [[Manual.TopicTree][]]
- [[Manual.DraValueID03][]]
- [[Manual.AppendixC][]]
- [[Manual.AppendixATJCAddendum][]]
- [[Manual.WebNotify][]]
- [[Manual.MeasureInformationFormTemplate][]]
- [[Manual.MeasureSetForm][]]
- [[Manual.ReleaseRecord0015PublishRecord][]]
- [[Manual.SupplementalMaterialTemplate][]]
- [[Manual.TransmissionDataProcessingFlowTJC][]]
- [[Manual.MeasureSet][]]
- [[Manual.AppendixStroke][]]
- [[Manual.ImpNoteAsValueID06][]]
- [[Manual.QuestionCategoryID39][]]
- [[Manual.ImpNoteAsValueID04][]]
- [[Manual.PopulationOptions][]]
- [[Manual.QuestionCategoryID48][]]
- [[Manual.DataCluster007][]]
- [[Manual.QuestionCategoryID04][]]
- [[Manual.AcknowledgementTJC][]]
- [[Manual.ReferencesHCSS][]]
- [[Manual.TransmissionChapterTJC][]]
- [[Manual.QuestionCategoryID61][]]
- [[Manual.ReleaseRecord0028PublishRecord][]]
- [[Manual.QuestionCategoryID30][]]
- [[Manual.SCR00001][]]
- [[Manual.DataElementEditTemplate][]]
- [[Manual.AdoptionStatus02][]]
- [[Manual.PublishedManuals][]]
- [[Manual.SCRDetailsID100003][]]
- [[Manual.DataCluster012][]]
- [[Manual.QuestionCategoryID29][]]
- [[Manual.SCR00002][]]
- [[Manual.QuestionCategoryID54][]]
- [[Manual.ReleaseRecord0020PublishRecord][]]
- [[Manual.WebAliasSearches][]]
- [[Manual.HelpGuideCoreMeasureSolutionExchange][]]
- [[Manual.Test2AppendixARef][]]
- [[Manual.TypeOfMeasure02][]]
- [[Manual.TypeOfMeasure][]]
- [[Manual.DataCluster010Form][]]
- [[Manual.PublishContribHistory][]]
- [[Manual.DataCluster008][]]
- [[Manual.DataCluster012Form][]]
- [[Manual.QuestionCategoryID16][]]
- [[Manual.DataCollectionApproachID03][]]
- [[Manual.IntroductionStroke][]]
- [[Manual.ReleaseRecord0029PublishRecord][]]
- [[Manual.QuestionCategoryID44][]]
- [[Manual.SCRDetailsID100001][]]
- [[Manual.IntroductionHCSS][]]
- [[Manual.SamplingChapterTJC][]]
- [[Manual.SpecificationChangeRequestDetailsForm][]]
- [[Manual.AppendixHCSS][]]
- [[Manual.AppendixFTJC][]]
- [[Manual.ImpNoteAsValueID01][]]
- [[Manual.AppendixATJC][]]
- [[Manual.QuestionCategoryID33][]]
- [[Manual.UseStatus01][]]
- [[Manual.QuestionCategoryID37][]]
- [[Manual.ImpNoteAsValueID02][]]
- [[Manual.DiagnosticImagingNuclearMedicine][]]
- [[Manual.WebSearch][]]
- [[Manual.ImprovementNotedAs][]]
- [[Manual.CoverPageTJC][]]
- [[Manual.SpecificationChangeRequest][]]
- [[Manual.QuestionCategoryID23][]]
- [[Manual.WebStatistics][]]
- [[Manual.GlossaryHCSS][]]
- [[Manual.QualityMeasureVerificationProcess][]]
- [[Manual.QuestionCategoryID06][]]
- [[Manual.CommentID10003][]]
- [[Manual.AppendixHTJC][]]
- [[Manual.DataCluster016][]]
- [[Manual.CommentID10004][]]
- [[Manual.FormAttributeTemplate][]]
- [[Manual.QuestionCategoryID12][]]
- [[Manual.RestrictedAccessMessage][]]
- [[Manual.DataElementForm][]]
- [[Manual.QuestionCategoryID55][]]
- [[Manual.FormAttributeForm][]]
- [[Manual.TypeOfMeasure04][]]
- [[Manual.DataCluster005Form][]]
- [[Manual.DataCluster003Form][]]
- [[Manual.QuestionCategoryID14][]]
- [[Manual.DataCluster010][]]
- [[Manual.DiagnosticImagingComputedTomography][]]
- [[Manual.WebHome][]]
- [[Manual.WebIndex][]]
- [[Manual.DataDictionaryIntroduction][]]
- [[Manual.QuestionCategory][]]
- [[Manual.DataCluster014][]]
- [[Manual.DataCluster005][]]
- [[Manual.StaffNavigationMenu][]]
- [[Manual.ReleaseRecord0021PublishRecord][]]
- [[Manual.WebTopicList][]]
- [[Manual.DataCluster002][]]
- [[Manual.DataCollectionHCSS][]]
- [[Manual.ReleaseRecord0018PublishRecord][]]
- [[Manual.QuestionCategoryID35][]]
- [[Manual.SupplementalMaterial][]]
- [[Manual.QuestionCategoryID40][]]
- [[Manual.AdoptionStatus][]]
- [[Manual.DataCluster011][]]
- [[Manual.DataElementTemplate][]]
- [[Manual.DiagnosticImagingHelp][]]
- [[Manual.QuestionCategoryID31][]]
- [[Manual.QuestionCategoryID00][]]
- [[Manual.QuestionCategoryID10][]]
- [[Manual.MeasureSetPrintPackage][]]
- [[Manual.HighReliabilityInfectionControlLTC][]]
- [[Manual.IntroductionPBM][]]
- [[Manual.PublishContribHistoryTest][]]
- [[Manual.DataCluster009Form][]]
- [[Manual.AppendixD][]]
- [[Manual.AcknowledgementPBM][]]
- [[Manual.Acknowledgement][]]
- [[Manual.ReleaseRecord0031PublishRecord][]]
- [[Manual.ReleaseRecord0026PublishRecord][]]
- [[Manual.QuestionCategoryID63][]]
- [[Manual.ReleaseRecord0008PublishRecord][]]
- [[Manual.QuestionCategoryID09][]]
- [[Manual.MeasureSetTemplate][]]
- [[Manual.CommentID10001][]]
- [[Manual.ReleaseRecord0030PublishRecord][]]
- [[Manual.ReleaseRecord0022PublishRecord][]]
- [[Manual.DiagnosticImagingMagneticResonance][]]
- [[Manual.DataCluster008Form][]]
- [[Manual.ImpNoteAsValueID07][]]
- [[Manual.QuestionCategoryID20][]]
- [[Manual.QuestionCategoryID51][]]
- [[Manual.DataCollectionStroke][]]
- [[Manual.TableofContentsStroke][]]
- [[Manual.DataCluster018][]]
- [[Manual.SamplingChapter][]]
- [[Manual.FormAttribute][]]
- [[Manual.QuestionCategoryID50][]]
- [[Manual.QuestionCategoryID07][]]
- [[Manual.RenderCreateNewSCRDetails][]]
- [[Manual.DataCluster014Form][]]
- [[Manual.PopulationOptionsID00][]]
- [[Manual.DiagnosticImagingFluoroscopy][]]
- [[Manual.MissingAndInvalidDataTJC][]]
- [[Manual.RelatedTopicsList][]]
- [[Manual.DraValueID02][]]
- [[Manual.ProphylacticAntibioticRegimenSelectionForSurgery][]]
- [[Manual.AppendixACAH][]]
- [[Manual.QuestionCategoryID27][]]
- [[Manual.SCR00003][]]
- [[Manual.ReleaseRecord0027PublishRecord][]]
- [[Manual.DataDictionaryIntroductionPBM][]]
- [[Manual.ChangesToManual][]]
- [[Manual.QuestionCategoryID42][]]
- [[Manual.DiagnosticComputedTomographyAltDisplay][]]
- [[Manual.UseStatus00][]]
- [[Manual.AppendixG][]]
- [[Manual.SpecificationChangeRequestDetails][]]
- [[Manual.SpecificationChangeRequestDetailsTemplate][]]
- [[Manual.DiagnosticImagingContributionSummary][]]
- [[Manual.AppendixATableMap][]]
- [[Manual.TopicClassification][]]
- [[Manual.TestPublishTopic][]]
- [[Manual.QuestionCategoryID19][]]
- [[Manual.AlgorithmTwo][]]
- [[Manual.QuestionCategoryID46][]]
- [[Manual.SamplingStroke][]]
- [[Manual.QuestionCategoryID59][]]
- [[Manual.QuestionCategoryID22][]]
- [[Manual.TypeOfMeasure01][]]
- [[Manual.DiagnosticImagingExpertPanel][]]
- [[Manual.DataCollectionToolsStroke][]]
- [[Manual.DataCollectionApproachID01][]]
- [[Manual.DevelopmentStatus][]]
- [[Manual.ListOfDataElements][]]
- [[Manual.ImportTableForm][]]
- [[Manual.WebRss][]]
- [[Manual.UsingTheManualTJC][]]
- [[Manual.TopicClassForm][]]
- [[Manual.DataDictionaryIntroductionTJC][]]
- [[Manual.ReferencesStroke][]]
- [[Manual.QuestionCategoryID02][]]
- IV Thrombolytic Therapy Prior to IA or Mechanical Reperfusion Therapy
- ABC/2 Estimate
- ABG Done
- ACEI Prescribed at Discharge
- ACEI Prescribed for LVSD in the Outpatient Setting
- ACEI or ARB for LVSD
- ACEI or ARB for LVSD
- AMI or HF patients prescribed ACEI or ARB for LVSD at discharge
- ARB Prescribed at Discharge
- ARB Prescribed for LVSD in the Outpatient Setting
- Active Clinical Staff
- Activity Recommendation Duration of Activity
- Activity Recommendation Intensity of Activity
- Activity Recommendation Type of Activity
- Activity Recommendations Document
- Acute Myocardial Infarction
- Admission Date
- Admission Date-Stroke
- Admission From Home
- Admission Screening for Violence Risk, Substance Use, Psychological Trauma History and Patient Strengths completed
- Admission Screening- Adolescent (13 through 17 years)
- Admission Screening- Adult (18 through 64 years)
- Admission Screening- Children (1 through 12 years)
- Admission Screening- Older Adult (≥65 years)
- Admission Screening- Overall Rate
- Admission Time
- Admission Type
- Admission to NICU
- Admit Decision Time to ED Departure Time for Admitted Patients
- Admitted for Elective Carotid Endarterectomy
- Admitting Diagnosis
- Adult Smoking Cessation Advice/Counseling
- Adult Smoking Cessation Advice/Counseling
- Adult Smoking Cessation Advice/Counseling
- Adult Smoking Counseling
- Adult Smoking Counseling-Stroke
- Adult Smoking History
- Adult Smoking History-Stroke
- Advance Directive Executed
- Advance Directive Executed
- Advanced Certification Heart Failure
- Advanced Certification Heart Failure Outpatient
- Age
- Age 18 or Greater
- Alcohol & Drug Use: Assessing Status After Discharge
- Alcohol & Other Drug Use Disorder Treatment Provided or Offered at Discharge
- Alcohol & Other Drug Use Disorder Treatment at Discharge
- Alcohol Use Brief Intervention
- Alcohol Use Brief Intervention Provided or Offered
- Alcohol Use Brief Intervention Provided or Offered
- Alcohol Use Screening
- Alcohol Use Status
- Alcohol and Other Drug Use Disorder Treatment fProvided or Offered at Discharge
- Alcohol or Drug Disorder
- Alcohol or Drug Use Status Post-Discharge (Not used in measure calculation)
- Aldosterone Receptor Antagonist Prescribed for LVSD in the Outpatient Setting
- Ambulation Device
- Ambulation Device Location
- Ambulation Device Location Other
- Ambulation Device Other
- Ambulation Device Required
- Anesthesia End Date
- Anesthesia End Time
- Anesthesia Start Date
- Anesthesia Start Time
- Anesthesia Type
- Another Source of Infection
- Antenatal Steroid Therapy Initiated
- Antenatal Steroids
- Antibiotic Administration Date
- Antibiotic Administration Route
- Antibiotic Administration Time
- Antibiotic Allergy
- Antibiotic Name
- Antibiotic Received
- Antibiotic Selection
- Antibiotic Timing
- Antibiotic Timing (Median)
- Antithrombotic Therapy Administered by End of Hospital Day Two
- Antithrombotic Therapy By End of Hospital Day Two
- Antithrombotic Therapy Prescribed at Discharge
- Appropriate Justification for Multiple Antipsychotic Medications
- Arrival Date
- Arrival Date
- Arrival Date-Stroke
- Arrival Time
- Arrival Time-Stroke
- Aspirin Prescribed at Discharge
- Aspirin Prescribed at Discharge
- Aspirin Received Within 24 Hours Before or After Hospital Arrival
- Aspirin at Arrival
- Aspirin at Arrival
- Aspirin at arrival for hospital inpatient and outpatient Emergency Department (ED) acute myocardial infarction (AMI) or probable cardiac chest pain patients
- Aspirin at arrival for inpatient AMI or probable cardiac chest pain patients
- Aspirin at arrival for outpatient ED AMI or probable cardiac chest pain patients
- Assessed for Rehabilitation
- Assessed for Rehabilitation Services
- Assessment - Bone Health Risk
- Assessment - Fatigue
- Assessment - Lymphedema
- Assessment - Menopausal Symptoms
- Assessment - Neuropathy
- Assessment - Pain
- Assessment - Psychosocial Distress
- Assessment - Sleep
- Assessment Tool
- Assessment for Chemotherapy Induced Nausea and Vomiting
- Assessment for Chemotherapy Induced Nausea and Vomiting
- Assessment for Distress
- Assessment for Fatigue
- Assessment for Sleep-Wake Disturbance
- Assessment in EMR
- Atrial Fibrillation
- Background Check
- Beta-Blocker Current Medication
- Beta-Blocker During Pregnancy
- Beta-Blocker Perioperative
- Beta-Blocker Prescribed at Discharge
- Beta-Blocker Prescribed at Discharge
- Beta-Blocker Received Within 24 Hours After Hospital Arrival
- Beta-Blocker Therapy (i.e., Bisoprolol, Carvedilol, or Sustained-Release Metoprolol Succinate for LVSD Prescribed at Discharge)
- Beta-Blocker at Arrival
- Birth Weight
- Birthdate
- Birthdate
- Bisoprolol, Carvedilol, or Sustained-Release Metoprolo Succinate Prescribed for LVSD at Discharge
- Bisoprolol, Carvedilol, or Sustained-Release Metoprolol Prescribed for LVSD in the Outpatient Setting
- Blood Administration Documentation
- Blood Administration Location
- Blood Bank Records
- Blood Culture Collected
- Blood Cultures Performed Within 24 Hours Prior to or 24 Hours After Hospital Arrival for Patients Who Were Transferred or Admitted to the ICU Within 24 Hours of Hospital Arrival
- Blood Cultures Performed in the Emergency Department Prior to Initial Antibiotic Received in Hospital
- Blood ID Number
- Blood Type Testing Ordered
- Bloodstream Infection Present on Admission
- Bone Mineral Density Test Performed in the 12 Months Prior to the Fracture
- Breast Cancer Care
- Breast Cancer Stage
- Breast Cancer Survivorship
- Breast Imaging
- Brief Intervention
- CMS Certification Number
- CMS Risk-Adjusted 30-Day Mortality
- CPT® Code
- CSF Prescribed
- Cardiac Arrest
- Cardiac Arrest Date
- Cardiac Arrest Event Number
- Cardiac Arrest Time
- Cardiac Resynchronization Therapy
- Cardiac Surgery Patients With Controlled 6 A.M. Postoperative Blood Glucose
- Care Transition Record Given to Patient/Caregiver
- Care Transition Record Transmitted
- Care Transition Record Transmitted
- Care Transition Record-Condition or Functional Status at Discharge
- Care Transition Record-Designated Patient Caregiver or Social Support
- Care Transition Record-Discharge Medications
- Care Transition Record-Follow-Up Treatment(s) and Service(s) Needed
- Care Transition Record-Location, Date, and Time of Post-Discharge Appointment
- Care Transition Record-Next Level of Care Provider Contact Information
- Care Transition Record-Procedures Performed During Hospitalization
- Care Transition Record-Reason for Hospitalization
- Care Transition Record-Treatment(s)/Service(s) Provided
- Case Identifier
- Central Line-Associated Bloodstream Infection Rate
- Cesarean Section
- Cesarean Section - 15 through 19 years
- Cesarean Section - 20 through 24 years
- Cesarean Section - 25 through 29 years
- Cesarean Section - 30 through 34 years
- Cesarean Section - 35 through 39 years
- Cesarean Section - 40 through 44 years
- Cesarean Section - 45 through 64 years
- Cesarean Section - 8 through 14 years
- Cesarean Section - Overall Rate
- Chemotherapy Cycle Number
- Chest X-Ray
- Childrens Asthma Care
- Cholesterol Reducing Therapy Prescribed at Discharge
- Cholesterol Reducing Therapy Prior To Hospitalization
- Clinical Indication for Plasma
- Clinical Indication for Platelets
- Clinical Indication for Prophylactic Platelets
- Clinical Indication for RBCs
- Clinical Staff
- Clinical Trial
- Clinical Trial - Osteo
- Code Status Order
- Code Status Order Date
- Code Status Order Time
- Cognitive Impairment
- Colony Stimulation Factors (CSF) Prescribed
- Colorectal Surgery Patients with Immediate Postoperative Normothermia
- Comatose
- Comfort Measures Only
- Comfort Measures Only
- Comfort Measures Only - Stroke
- Competency
- Completeness of Personnel File
- Comprehensive Stroke
- Compromised
- Condition Changed
- Congenital Anomalies
- Consent Addressed Transfusion Benefits
- Consent Addressed Transfusion Risks
- Continuing Assessment
- Continuing Assessment - Distress
- Continuing Assessment - Fatigue
- Continuing Assessment - Overall Rate
- Continuing Assessment - Sleep-Wake Disturbance
- Continuing Care Plan-Discharge Medications
- Continuing Care Plan-Next Level of Care
- Continuing Care Plan-Principal Discharge Diagnosis
- Continuing Care Plan-Reason for Hospitalization
- Contraindication to Systemic Corticosteroids
- Contraindication Status - Head of Bed Elevation
- Contraindication Status - SUD Prophylaxis
- Contraindication to Aspirin at Discharge
- Contraindication to Aspirin on Arrival
- Contraindication to Beta-Blocker - Perioperative
- Contraindication to Beta-Blocker at Discharge
- Contraindication to Beta-Blocker on Arrival
- Contraindication to Both ACEI and ARB at Discharge
- Contraindication to Relievers
- Contraindication to VTE Prophylaxis
- Coordination of Care
- Critical Access Hospital
- DVT Prophylaxis Initiated by End of Hospital Day 2
- DXA Scan Ordered or Performed Prior to Discharge
- Data Source
- Date
- Date IV Thrombolytic Therapy Administered At This Hospital
- Date Last Known Well
- Date Therapeutic Hypothermia Ended
- Date Therapeutic Hypothermia Initiated
- Date Therapeutic Hypothermia Ordered
- Date of Infection
- Death Among Surgical Inpatients with Treatable Serious Complications
- Diagnostic Uncertainty
- Direct Admission
- Discharge Code
- Discharge Date
- Discharge Date-SCA
- Discharge Disposition
- Discharge Disposition
- Discharge Instructions
- Discharge Instructions Address Activity
- Discharge Instructions Address Diet
- Discharge Instructions Address Follow-up
- Discharge Instructions Address Medications
- Discharge Instructions Address Symptoms Worsening
- Discharge Instructions Address Weight Monitoring
- Discharge Instructions Emergency Department
- Discharge Status
- Discharge Status
- Discharge Status-Stroke
- Discharge Time
- Discharge Time
- Discharged Home From The ED
- Discharged on Antithrombotic Therapy
- Discharged on Cholesterol Reducing Medication
- Discussion of Advance Directives/Advance Care Planning
- Discussion of Advance Directives/Advance Care Planning
- Disease Specific Instrument
- Distress
- Distress Improvement
- Do Not Return - Clinical
- Do Not Return - Clinical
- Do Not Return - Professional
- Do Not Return - Professional
- Do Not Return Occurrence Identifier
- Door to Diagnostic Evaluation by a Qualified Medical Personnel for hospital inpatients and outpatients seen in the emergency department (ED)
- Door to Diagnostic Evaluation by a Qualified Medical Personnel for hospital inpatients seen in the ED
- Door to Diagnostic Evaluation by a Qualified Medical Personnel for hospital outpatients seen in the ED
- Dysphagia Screen
- Dysphagia Screening
- E/M Code
- ECG
- ECG Date
- ECG Time
- ED Departure Date
- ED Departure Time
- ED Patient
- ED Patient
- Education Addresses Activation of Emergency Medical System
- Education Addresses Follow-up After Discharge
- Education Addresses Medication Prescribed
- Education Addresses Risk Factors for Stroke
- Education Addresses Warning Signs and Symptoms of Stroke
- Education on Community Resources
- Education on Diet
- Education on Exercise
- Education on Late Effects
- Education on Lymphedema
- Education on Neutropenia Precautions
- Education on Recurrence
- Elective Carotid Intervention
- Elective Delivery
- Elective Surgery
- Emergency Department
- Emergency Order Date
- Emergency Order Time
- Emergency Transfusion
- Emergency Transfusion Date
- Emergency Transfusion Time
- Emetogenic Agents
- Endotracheal Intubation Confirmation Date
- Endotracheal Intubation Confirmation Time
- Endotracheal Intubation Date
- Endotracheal Intubation Time
- Endotracheal Tube Insertion
- Evaluation of LVS Function
- Event Date
- Event Type
- Exclusive Breast Milk Feeding
- Exclusive Breast Milk Feeding
- Exclusive Breast Milk Feeding Considering Mother's Initial Feeding Plan
- Exercise Program
- FDA-approved Pharmacotherapy for Treatment of Osteoporosis
- Fall Assessment Education
- Fall Date
- Fall RA Disciplines
- Fall RA Elements
- Fall RA Score
- Fall Risk Assessment
- Fall Risk Indicators
- Fall general information
- Fall resulted in injury
- Falls Medications
- Falls Project CTHC
- Falls with Injury
- Fatigue Improvement
- Fatigue Level Begin
- Fatigue Level End
- Fibrinolytic Administration
- Fibrinolytic Administration Date
- Fibrinolytic Administration Time
- Fibrinolytic Therapy Received Within 30 Minutes
- Fibrinolytic Therapy Received Within 30 Minutes of Hospital Arrival
- Fibrinolytic therapy received within 30 minutes of hospital arrival for hospital inpatient AMI patients with ST-segment elevation or LBBB.
- Fibrinolytic therapy received within 30 minutes of hospital arrival for hospital inpatient and outpatient Emergency Department (ED) acute myocardial infarction (AMI) patients with ST-segment elevation or LBBB.
- Fibrinolytic therapy received within 30 minutes of hospital arrival for hospital outpatient ED AMI patients with ST-segment elevation or LBBB.
- Final Treatment Date
- First Chemotherapy Date
- First Defibrillation Shock Date
- First Defibrillation Shock Time
- First In-Hospital LDL-Cholesterol Qualitative Description
- First In-Hospital LDL-Cholesterol Value
- First Name
- First PCI Date
- First PCI Time
- First Pass Date
- First Pass Time
- First Pass of a Mechanical Reperfusion Device
- Follow Up Care
- Follow Up Care - Breast Imaging
- Follow Up Care - Composite Rate
- Follow Up Care - Coordination of Care
- Follow Up Care - LVEF Assessment
- Follow Up Care - Pelvic Exam
- Follow-up Contact
- Follow-up Contact Date
- Gestational Age
- Glucose POD 1
- Glucose POD 2
- Goal Attainment
- Goal Setting
- Goals Collaborative
- Head CT or MRI Scan Interpretation Date
- Head CT or MRI Scan Interpretation Time
- Head CT or MRI Scan Order
- Head CT or MRI scan results for acute ischemic stroke or hemorrhagic stroke patients who received head CT or MRI scan interpretation within 45 minutes of ED arrival for hospital inpatients
- Head CT or MRI scan results for acute ischemic stroke or hemorrhagic stroke patients who received head CT or MRI scan interpretation within 45 minutes of ED arrival for hospital inpatients and outpatients
- Head CT or MRI scan results for acute ischemic stroke or hemorrhagic stroke patients who received head CT or MRI scan interpretation within 45 minutes of ED arrival for hospital outpatients
- Head of Bed Elevated
- Health Care Organization Identifier
- Health Care Staffing Services
- Health Care-Associated Bloodstream Infections in Newborns
- Health Status
- Healthcare Associated PN
- Heart Failure
- Hemorrhagic Transformation (Overall Rate)
- Hemorrhagic Transformation for Patients Treated with Intra-Arterial (IA) Thrombolytic (t-PA) Therapy or Mechanical Endovascular Reperfusion Therapy
- Hemorrhagic Transformation for Patients Treated with Intra-Venous (IV) Thrombolytic (t-PA) Therapy Only
- Highest NIHSS Score Documented Within 36 Hours Following IA t-PA or MER Initiation
- Highest NIHSS Score Documented Within 36 Hours Following IV Thrombolytic Initiation
- Hispanic Ethnicity
- Home Management Plan of Care (HMPC) Document Given to Patient/Caregiver
- Home Management Plan of Care Document Addresses Arrangements for Follow-up Care
- Home Management Plan of Care Document Addresses Environmental Control and Control of Other Triggers
- Home Management Plan of Care Document Addresses Methods and Timing of Rescue Actions
- Home Management Plan of Care Document Addresses Use of Controllers
- Home Management Plan of Care Document Addresses Use of Relievers
- Home Management Plan of Care Document Given to Patient/Caregiver
- Home Management Plan of Care Document Present
- Hospital Based Inpatient Psychiatric Services
- Hospital Outpatient ACEI or ARB Prescribed for LVSD
- Hospital Outpatient Activity Recommendations
- Hospital Outpatient Advance Directive Executed
- Hospital Outpatient Aldosterone Receptor Antagonists Prescribed for LVSD
- Hospital Outpatient Beta-Blocker Therapy (i.e., Bisoprolol, Carvedilol, or Sustained-Release Metoprolol Succinate) Prescribed for LVSD
- Hospital Outpatient Cardiac Resynchronization Therapy (CRT, CRT with pacing CRT-P, CRT with defribrillator CRT-D)
- Hospital Outpatient Department
- Hospital Outpatient Discussion of Advance Directives/Advance Care Planning
- Hospital Outpatient ICD Counseling for LVSD
- Hosptial Outpatient New York Heart Association (NYHA) Classification Assessment
- Hours Worked
- Hours of physical restraint use
- Hours of seclusion use
- Hunt and Hess Scale Performed for SAH Patients
- IA Route of t-PA Administration
- IA Thrombolytic Initiation
- IA Thrombolytic Initiation Date
- IA Thrombolytic Initiation Time
- IA t-PA or MER Initiation Date
- IA t-PA or MER Initiation Time
- ICD Counseling
- ICD Population Size
- ICD-10-CM Other Diagnosis Codes
- ICD-10-CM Principal Diagnosis Code
- ICD-10-PCS Other Procedure Codes
- ICD-10-PCS Other Procedure Dates
- ICD-10-PCS Principal Procedure Code
- ICD-10-PCS Principal Procedure Date
- ICD-9-CM Diagnosis Code
- ICD-9-CM Other Diagnosis Codes
- ICD-9-CM Other Procedure Codes
- ICD-9-CM Other Procedure Dates
- ICD-9-CM Other Procedure Times
- ICD-9-CM Principal Diagnosis Code
- ICD-9-CM Principal Procedure Code
- ICD-9-CM Principal Procedure Date
- ICD-9-CM Principal Procedure Time
- ICH Score Performed for ICH Patients
- ICU Admission Date
- ICU Admission Time
- ICU Admission or Transfer
- ICU Admitting Diagnosis
- ICU Discharge Date
- ICU Discharge Time
- ICU Readmit
- ICU VTE Prophylaxis
- ICU VTE Prophylaxis
- ICU VTE Prophylaxis Date
- INR Value < 1.4
- INR Value < 1.4 Date
- INR Value < 1.4 Time
- INR Value > 1.4
- IV Thrombolytic Initiation Date
- IV Thrombolytic Initiation Time
- IV Thrombolytic Therapy Administered
- Identified Pathogen
- Immunization
- Implanted Device
- In-Hospital LDL-Cholesterol Test
- Incidence of Potentially Preventable Hospital-Acquired VTE
- Infection Prior to Anesthesia
- Influenza Immunization
- Influenza Vaccination
- Influenza Vaccination Status
- Information Addressed Risks, Benefits and Alternatives to Transfusion
- Initial Antibiotic Received Within 4 Hours of Hospital Arrival
- Initial Antibiotic Received Within 6 Hours of Hospital Arrival (NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE)
- Initial Antibiotic Received Within 8 Hours of Hospital Arrival - RETIRED
- Initial Antibiotic Selection for Community-Acquired Pneumonia (CAP in Immunocompetent Patients Intensive Care Unit (ICU) Patients)
- Initial Antibiotic Selection for Community-Acquired Pneumonia (CAP in Immunocompetent Patients Non ICU Patients)
- Initial Antibiotic Selection for Community-Acquired Pneumonia (CAP in Immunocompetent Patients)
- Initial Antibiotic Selection for Community-Acquired Pneumonia (CAP) in Immunocompetent Patients
- Initial Blood Culture Collection Date
- Initial Blood Culture Collection Time
- Initial Blood Glucose Value at Hospital Arrival
- Initial Blood Pressure at Hospital Arrival
- Initial ECG Interpretation
- Initial Hunt and Hess Scale Date
- Initial Hunt and Hess Scale Performed
- Initial Hunt and Hess Scale Time
- Initial ICH Score Date
- Initial ICH Score Performed
- Initial ICH Score Time
- Initial NIHSS Score Date
- Initial NIHSS Score Performed
- Initial NIHSS Score Time
- Initial NIHSS Score at Hospital Arrival
- Initial Patient Population Size Medicare Only
- Initial Patient Population Size Non-Medicare Only
- Initial Platelet Count at Hospital Arrival
- Initial Rhythm
- Initiation of Therapeutic Hypothermia
- Inpatient Mortality
- Inpatient Neonatal Mortality
- Instructions on Hand Washing
- Instructions to Contact Provider
- Intervention for Bone Health Risk
- Intervention for Distress
- Intervention for Distress
- Intervention for Fatigue
- Intervention for Fatigue
- Intervention for Lymphedema
- Intervention for Menopausal Symptoms
- Intervention for Neuropathy
- Intervention for Pain
- Intervention for Psychosocial Distress
- Intervention for Sleep
- Intervention for Sleep -Wake Disturbance
- Intervention for Sleep-Wake Disturbance
- Intubated
- Job Appropriate Credentials
- Joint Revision
- LDL ≥ 100 mg/dL
- LDL Cholesterol Assessment (Optional Test Measure)
- LDL-c Less Than 100 mg/dL
- LVEF Assessment
- LVF Assessment
- LVSD
- LVSD < 40%
- LVSD of < 35%
- Labor
- Laboratory Investigation for Secondary Causes of Osteoporosis
- Laboratory Testing Performed in the Prior 12 Months
- Laboratory Tests Ordered or Performed Prior to Discharge
- Laparoscope
- Last Known Well
- Last Name
- Left Bundle Branch Block (LBBB) on ECG
- Left Ventricular Assist, Device Biventricular Assist Device
- Lipid-Lowering Agent Prescribed at Discharge
- Lipid-Lowering Therapy at Discharge (Optional Test Measure)
- Location of Fall
- Location of Fall Other
- Maintenance of Thermoregulation in Therapeutic Hypothermia
- Measure Category Assignment
- Measure Category Assignment
- Measure Set
- Measurement Value
- Median Time from ED Arrival to ED Departure for Admitted ED Patients
- Median Time to ECG
- Median Time to ECG for hospital inpatient AMI or probable cardiac chest pain patients
- Median Time to ECG for hospital inpatient and outpatient acute myocardial infarction (AMI) and probable cardiac chest pain patients
- Median Time to ECG for hospital outpatient AMI or probable cardiac chest pain patients
- Median Time to Fibrinolysis
- Median Time to Fibrinolysis
- Median Time to INR Reversal
- Median Time to Primary PCI
- Median Time to Revascularization
- Median Time to Transfer to Another Facility for Acute Coronary Intervention
- Median Time to Transfer to Another Facility for Coronary Intervention
- Median Time to Treatment with a Procoagulant Reversal Agent
- Medication Bedtime
- Medication Change
- Medication Education
- Methods of Intubation Confirmation
- Minutes of Physical Restraint
- Minutes of Seclusion
- Modified Rankin Score (mRS at 90 Days)
- Modified Rankin Score (mRS)
- Modified Rankin Score (mRS) Date
- Multiple Antipsychotic Medications at Discharge with Appropriate Justification- Adolescent (13 through 17 years)
- Multiple Antipsychotic Medications at Discharge with Appropriate Justification- Adult (18 through 64 years)
- Multiple Antipsychotic Medications at Discharge with Appropriate Justification- Children (1 through 12 years)
- Multiple Antipsychotic Medications at Discharge with Appropriate Justification- Older Adult (≥ 65 years)
- Multiple Antipsychotic Medications at Discharge with Appropriate Justification- Overall Rate
- Multiple Antipsychotic Medications at Discharge- Adolescent (13 through 17 years)
- Multiple Antipsychotic Medications at Discharge- Adult (18 through 64 years)
- Multiple Antipsychotic Medications at Discharge- Children (1 through 12 years)
- Multiple Antipsychotic Medications at Discharge- Older Adult (≥ 65 years)
- Multiple Antipsychotic Medications at Discharge- Overall Rate
- Multiple Births
- Myelosuppressive Chemotherapy
- NIHSS Score Documented Closest to IA t-PA or MER Initiation
- NIHSS Score Documented Closest to IV Thrombolytic Initiation
- NPO (Nothing by Mouth) For Entire Hospital Stay
- National Institutes of Health Stroke Scale (NIHSS Score Performed for Ischemic Stroke Patients)
- National Provider Identifier
- Neuraxial Anesthesia
- Neutropenia Risk Cycle
- New York Heart Association (NYHA) Classification
- New data element
- Newborn Admission Source
- Nimodipine Administration
- Nimodipine Administration Date
- Nimodipine Administration Time
- Nimodipine Treatment Administered
- Non-Primary PCI
- Number of Antipsychotic Medications Prescribed at Discharge
- Number of Cases with UTD Allowable Values
- Number of Rejected Cases
- Nursing Care Hours per Patient Day
- Nursing-Sensitive Care
- On FDA-approved Pharmacotherapy for Treatment of Osteoporosis Prior to Fracture
- Optimal Medication Management
- Oral Administration of Vitamin D
- Oral Antibiotics
- Osteoporosis
- Other Fracture Risk Assessment Method Ordered or Performed Prior to Discharge
- Other Surgeries
- Outpatient Encounter Date
- Parity
- Patient Ambulatory at End of Hospital Day Two
- Patient Blood Management
- Patient Discharged on Anticoagulation Therapy
- Patient Falls
- Patient HIC#
- Patient ID
- Patient ID Verification
- Patient Identifier
- Patient Location
- Patient Referral to Next Level of Care Provider
- Patient Room Circumstances
- Patient Strengths
- Patients discharged on multiple antipsychotic medications
- Patients discharged on multiple antipsychotic medications with appropriate justification
- Patients with Atrial Fibrillation Receiving Anticoagulation Therapy
- Payment Source
- Pelvic Exam
- Performance Measure Identifier
- Performance Measurement System Identifier
- Perinatal Care
- Perioperative Death
- Personnel File Record Identifier
- Physical Restraint- Adolescent (13 through 17 years)
- Physical Restraint- Adult (18 through 64 years)
- Physical Restraint- Children (1 through 12 years)
- Physical Restraint- Older Adult (≥ 65 years)
- Physical Restraint- Overall Rate
- Physician 1
- Physician 2
- Plan for LDL-Cholesterol Test
- Plasma ID
- Plasma Event Total Doses
- Plasma Transfusion Indication
- Platelet ID
- Platelet Event Total Doses
- Platelet Transfusion Indication
- Pneumococcal Immunization Overall Rate
- Pneumococcal Vaccination
- Pneumococcal Vaccination Status
- Pneumonia
- Pneumonia Diagnosis: ED/Direct Admit
- Point of Origin for Admission or Visit
- Point of Origin for Admission or Visit
- Point of Origin for Admission or Visit-Stroke
- Portugal ICU
- Portugal ICU 1
- Portugal ICU 2
- Portugal ICU 3
- Portugal ICU 6
- Portugal SCIP
- Portugal SCIP-INF1
- Portugal SCIP-INF2
- Portugal SCIP-INF3
- Portugal SCIP-VTE1
- Portugal SCIP-VTE2
- Positive Brain Image
- Positive Brain Image Date
- Positive Brain Image Time
- Post Discharge Continuing Care Plan Transmitted - Adolescent (13 through 17 years)
- Post Discharge Continuing Care Plan Transmitted - Adult (18 through 64 years)
- Post Discharge Continuing Care Plan Transmitted - Children (1 through 12 years)
- Post Discharge Continuing Care Plan Transmitted - Older Adult (≥65 years)
- Post Discharge Continuing Care Plan Transmitted- Overall Rate
- Post Discharge Continuing Care Plan- Adolescent (13 through 17 years)
- Post Discharge Continuing Care Plan- Adult (18 through 64 years)
- Post Discharge Continuing Care Plan- Children (1 through 12 years)
- Post Discharge Continuing Care Plan- Older Adult (≥ 65 years)
- Post Discharge Continuing Care Plan- Overall Rate
- Post discharge continuing care plan created
- Post discharge continuing care plan transmitted to next level of care provider upon discharge
- Post-Discharge Appointment Scheduled Within 7 Days
- Post-Discharge Appointment for Heart Failure Patients
- Post-Discharge Evaluation Conducted Within 72 Hours
- Post-Discharge Evaluation for Heart Failure Patients
- Post-Treatment Education
- Post-Treatment Education - Community Resources
- Post-Treatment Education - Composite Rate
- Post-Treatment Education - Diet
- Post-Treatment Education - Exercise
- Post-Treatment Education - Late Effects
- Post-Treatment Education - Lymphedema
- Post-Treatment Education - Recurrence
- Post-Treatment Thrombolysis in Cerebral Infarction (TICI) Reperfusion Grade
- Postal Code
- Postoperative Infections
- Practice Environmental Scale-Nursing Work Index
- Pre-Arrival LDL-Cholesterol Qualitative Description
- Pre-Arrival LDL-Cholesterol Test
- Pre-Arrival LDL-Cholesterol Value
- Pre-Arrival Lipid-Lowering Agent
- Pre-Treatment Assessment
- Pre-Treatment Assessment - Distress
- Pre-Treatment Assessment - Fatigue
- Pre-Treatment Assessment - Overall Rate
- Pre-Treatment Assessment - Sleep-Wake Disturbance
- Pre-transfusion Hematocrit Result
- Pre-transfusion Hemoglobin
- Pre-transfusion Hemoglobin
- Pre-transfusion Hemoglobin Result
- Pre-transfusion INR Result
- Pre-transfusion Laboratory Testing
- Pre-transfusion PT/INR
- Pre-transfusion Platelet Count
- Pre-transfusion Platelet Count Result
- Pre-transfusion Platelet Testing
- Preadmission Oral Anticoagulation Therapy
- Preadmission Warfarin
- Predicted Value
- Pregnancy and Related Conditions
- Preoperative Anemia Screening
- Preoperative Anemia Screening
- Preoperative Anemia Screening Hematocrit Result
- Preoperative Anemia Screening Hemoglobin Result
- Preoperative Anemia Screening Result Date
- Preoperative Blood Type Testing
- Preoperative Blood Type Testing and Antibody Screening
- Preoperative Hair Removal
- Prescription for Alcohol or Drug Disorder Medication
- Prescription for Tobacco Cessation Medication
- Pressure Ulcer Prevalence
- Primary PCI Received Within 90 Minutes of Hospital Arrival
- Prior Diagnosis of Osteoporosis
- Prior Uterine Surgery
- Probable Cardiac Chest Pain
- Procoagulant Reversal Agent Initiation
- Procoagulant Reversal Agent Initiation Date
- Procoagulant Reversal Agent Initiation Time
- Procoagulant Reversal Agent Initiation for Intracerebral Hemorrhage (ICH )
- Progress Toward Goals
- Prophylactic Antibiotic Received Within One Hour Prior to Surgical Incision
- Prophylactic Antibiotic Received Within One Hour Prior to Surgical Incision - CABG
- Prophylactic Antibiotic Received Within One Hour Prior to Surgical Incision - Colon Surgery
- Prophylactic Antibiotic Received Within One Hour Prior to Surgical Incision - Hip Arthroplasty
- Prophylactic Antibiotic Received Within One Hour Prior to Surgical Incision - Hysterectomy
- Prophylactic Antibiotic Received Within One Hour Prior to Surgical Incision - Knee Arthroplasty
- Prophylactic Antibiotic Received Within One Hour Prior to Surgical Incision - Other Cardiac Surgery
- Prophylactic Antibiotic Received Within One Hour Prior to Surgical Incision - Overall Rate
- Prophylactic Antibiotic Received Within One Hour Prior to Surgical Incision - Vascular Surgery
- Prophylactic Antibiotic Selection for Surgical Patients
- Prophylactic Antibiotic Selection for Surgical Patients - CABG
- Prophylactic Antibiotic Selection for Surgical Patients - Colon Surgery
- Prophylactic Antibiotic Selection for Surgical Patients - Hip Arthroplasty
- Prophylactic Antibiotic Selection for Surgical Patients - Hysterectomy
- Prophylactic Antibiotic Selection for Surgical Patients - Knee Arthroplasty
- Prophylactic Antibiotic Selection for Surgical Patients - Other Cardiac Surgery
- Prophylactic Antibiotic Selection for Surgical Patients - Overall Rate
- Prophylactic Antibiotic Selection for Surgical Patients - Vascular Surgery
- Prophylactic Antibiotics Discontinued Within 24 Hours After Surgery End Time
- Prophylactic Antibiotics Discontinued Within 24 Hours After Surgery End Time - Colon Surgery
- Prophylactic Antibiotics Discontinued Within 24 Hours After Surgery End Time - Hip Arthroplasty
- Prophylactic Antibiotics Discontinued Within 24 Hours After Surgery End Time - Knee Arthroplasty
- Prophylactic Antibiotics Discontinued Within 24 Hours After Surgery End Time - Overall Rate
- Prophylactic Antibiotics Discontinued Within 24 Hours After Surgery End Time - Vascular Surgery
- Prophylactic Antibiotics Discontinued Within 24 Hours After Surgery End Time Hysterectomy
- Prophylactic Antibiotics Discontinued Within 48 Hours After Surgery End Time - Other Cardiac Surgery
- Prophylactic Antibiotics Discontinued Within 48 Hours After Surgery End Time CABG
- Provider Contact Date
- Provider Contact Time
- Provider ID
- Provider ID
- Proximal or Distal Occlusion
- Pseudomonas Risk
- Psychiatric Care Setting
- Psychiatric Inpatient Days - Medicare Only
- Psychiatric Inpatient Days-Non-Medicare Only
- Psychological Trauma History
- Psychosocial Distress Level Begin
- Psychosocial Distress Level End
- Pulse Oximetry Done
- RBC Event Total Doses
- RBC ID
- RBC Transfusion Indication
- RBC Unit Exclusions
- Race
- Re-Assessment for Distress
- Re-Assessment for Fatigue
- Re-Assessment for Sleep-Wake Disturbance
- Reason for Delay in Fibrinolytic Therapy
- Reason for Delay in PCI
- Reason for Early Discontinuation of Therapeutic Hypothermia
- Reason for No ACEI and No ARB Prescribed for LVSD in Outpatient Setting
- Reason for No ACEI and No ARB at Discharge
- Reason for No Activity Recommendations in the Outpatient Setting
- Reason for No Aldosterone Receptor Antagonist Prescribed for LVSD in the Outpatient Setting
- Reason for No Aspirin at Discharge
- Reason for No Aspirin on Arrival
- Reason for No Bisoprolol, Carvedilol, or Sustained-Release Metoprolol Prescribed for LVSD in the Outpatient Setting
- Reason for No Bisoprolol, Carvedilol, or Sustained-Release Metoprolol Succinate Prescribed for LVSD at Discharge
- Reason for No Cardiac Resynchronization Therapy in the Outpatient Setting
- Reason for No DXA Scan
- Reason for No FDA-approved Pharmacotherapy for Treatment of Osteoporosis
- Reason for No ICD Counseling in the Outpatient Setting
- Reason for No LDL-Cholesterol Testing
- Reason for No Lipid-Lowering Therapy
- Reason for No Post-Discharge Appointment Within 7 Days
- Reason for No Preoperative Anemia Screening
- Reason for No Tobacco Cessation Medication During the Hospital Stay
- Reason for No Tobacco Cessation Medication at Discharge
- Reason for No VTE Prophylaxis - ICU Admission
- Reason for Not Administering Nimodipine Treatment
- Reason for Not Administering Fibrinolytic Therapy
- Reason for Not Administering Therapeutic Hypothermia
- Reason for Not Administering VTE Prophylaxis
- Reason for Not Administering a Procoagulant Reversal Agent
- Reason for Not Exclusively Feeding Breast Milk
- Reason for Not Initiating Antenatal Steroid Therapy
- Reason for Not Prescribing CSF
- Reason for Not Prescribing Statin Medication at Discharge
- Reason for Not Recommending Exercise
- Reason for Transfer
- Reason for Transfer Out Prior to Therapeutic Hypothermia
- Reasons to Extend Antibiotics
- Referral for Addictions Treatment
- Referral for Outpatient Tobacco Cessation Counseling
- Relievers Administered
- Relievers for Inpatient Asthma
- Relievers for Inpatient Asthma (age 13 through 17 years)
- Relievers for Inpatient Asthma (age 2 through 17 years) Overall Rate
- Relievers for Inpatient Asthma (age 2 through 4 years)
- Relievers for Inpatient Asthma (age 5 through 12 years)
- Report Period
- Restraint Prevalence (vest and limb)
- Return of Spontaneous Circulation
- Return of Spontaneous Circulation
- Risk Assessment/Treatment After Fracture
- Risk Factors for Drug-Resistant Pneumococcus
- Risk Indicator Reason
- Sample
- Sample Size Medicare Only
- Sample Size Non-Medicare Only
- Sampling Frequency
- Seclusion- Adolescent (13 through 17 years)
- Seclusion- Adult (18 through 64 years)
- Seclusion- Children (1 through 12 years)
- Seclusion- Older Adult (≥ 65 years)
- Seclusion- Overall Rate
- Severity Measurement Performed for SAH and ICH Patients (Overall Rate)
- Sex
- Site of Primary Vessel Occlusion
- Skill Mix
- Sleep-Wake Disturbance
- Smoking Cessation / Advice / Counseling
- Smoking Cessation Counseling for Acute Myocardial Infarction
- Smoking Cessation Counseling for Heart Failure
- Smoking Cessation Counseling for Pneumonia
- Specified Laboratory Tests
- Spontaneous Rupture of Membranes
- Statin Medication Prescribed at Discharge
- Statin Prescribed at Discharge
- Stress Ulcer Disease (SUD) Prophylaxis Administered
- Stroke Education
- Stroke Performance Measures
- Substance Use
- Substance Use Measures
- Sudden Cardiac Arrest
- Surgery End Date
- Surgery End Date - ICU Admission
- Surgery End Date - ICU Admission PRIOR TO
- Surgery End Time
- Surgery Patients Who Received Appropriate Venous Thromboembolism Prophylaxis Within 24 Hours Prior to Surgery to 24 Hours After Surgery
- Surgery Patients on Beta-Blocker Therapy Prior to Admission Who Received a Beta-Blocker During the Perioperative Period
- Surgery Patients with Appropriate Hair Removal
- Surgery Patients with Recommended Venous Thromboembolism Prophylaxis Ordered
- Surgery Scheduled Timeframe
- Surgery Start Date
- Surgery Start Time
- Surgical Care Improvement Project
- Surgical Incision Date
- Surgical Incision Time
- Surgical Procedure
- Surgical Procedure - ICU Admission
- Surgical Procedure - ICU Admission PRIOR TO
- Survivorship Visits
- Symptom - Bone Health Risk
- Symptom - Fatigue
- Symptom - Lymphedema
- Symptom - Menopausal
- Symptom - Neuropathy
- Symptom - Pain
- Symptom - Psychosocial Distress
- Symptom - Sleep
- Symptom Assessment
- Symptom Assessment - Bone Health Risk
- Symptom Assessment - Composite Rate
- Symptom Assessment - Fatigue
- Symptom Assessment - Lymphedema
- Symptom Assessment - Menopausal
- Symptom Assessment - Neuropathy
- Symptom Assessment - Pain
- Symptom Assessment - Psychosocial Distress
- Symptom Assessment - Sleep
- Symptom Intervention
- Symptom Intervention - Bone Health Risk
- Symptom Intervention - Composite Rate
- Symptom Intervention - Fatigue
- Symptom Intervention - Lymphedema
- Symptom Intervention - Menopausal
- Symptom Intervention - Neuropathy
- Symptom Intervention - Pain
- Symptom Intervention - Psychosocial Distress
- Symptom Intervention - Sleep
- Systemic Corticosteroids Administered
- Systemic Corticosteroids for Inpatient Asthma
- Systemic Corticosteroids for Inpatient Asthma (age 13 through 17 years)
- Systemic Corticosteroids for Inpatient Asthma (age 2 through 17 years) Overall Rate
- Systemic Corticosteroids for Inpatient Asthma (age 2 through 4 years)
- Systemic Corticosteroids for Inpatient Asthma (age 5 through 12 years)
- Temperature Value
- Test New Set
- Therapeutic Hypothermia Initiated
- Thermoregulation Maintained
- Third or Fourth Degree Laceration
- Thrombolysis in Cerebral Infarction (TICI Post-Treatment Reperfusion Grade)
- Thrombolytic Therapy Administered
- Tici reprufusion
- Time IV Thrombolytic Therapy Administered at This Hospital
- Time Last Known Well
- Time Therapeutic Hypothermia Ended
- Time Therapeutic Hypothermia Initiated
- Time Therapeutic Hypothermia Ordered
- Timeliness of First Defibrillation Attempt
- Timely Confirmation of Correct Endotracheal Tube
- Tobacco Treatment Measures
- Tobacco Use Screening
- Tobacco Use Status
- Tobacco Use Status Post-Discharge (Not used in measure calculation)
- Tobacco Use Treatment
- Tobacco Use Treatment
- Tobacco Use Treatment FDA-Approved Cessation Medication
- Tobacco Use Treatment Practical Counseling
- Tobacco Use Treatment Provided or Offered
- Tobacco Use Treatment Provided or Offered
- Tobacco Use Treatment Provided or Offered at Discharge
- Tobacco Use Treatment Provided or Offered at Discharge
- Tobacco Use Treatment at Discharge
- Tobacco Use: Assessing Status after Discharge
- Total Leave Days - Medicare Only
- Total Leave Days-Non-Medicare Only
- Transfer From Another ED
- Transfer From Another Hospital or ASC
- Transfer for Acute Coronary Intervention
- Transferred From or Expired in Emergency Department
- Transfusion Consent
- Transfusion Consent
- Transfusion Order
- Transfusion Start Date
- Transfusion Start Time
- Transfusion Type
- Treatment - Bilateral Mastectomy
- Treatment - Bone Health Risk
- Treatment - Breast Conserving
- Treatment - Menopause Inducer
- Treatment - Neuropathy Causing
- Treatment - Surgery or Radiation
- Treatment - Tamoxifen
- Treatment - Trastuzumab
- Type of Admission ICU
- UPSIDE - Debrief
- UPSIDE Bilateral Procedure
- UPSIDE Confederate
- UPSIDE Debrief Notes
- UPSIDE Describe Result
- UPSIDE Procedure
- UPSIDE Test Date
- UPSIDE Test Result
- UPSIDE Test Scenario
- Underlying Cause of Osteoporosis
- Unique Blinded Case Identifier
- Unique Blinded Health Care Organization Identifier
- Universal Protocol Simulation Implementation and Defect Evaluation
- Urinary Catheter-Associated Urinary Tract Infection Rate
- VBAC
- VTE Discharge Instructions
- VTE Patients Receiving UFH with Dosages/Platelet Count Monitoring by Protocol or Nomogram
- VTE Patients with Anticoagulation Overlap Therapy
- VTE Prophylaxis
- VTE Prophylaxis
- VTE Timely
- Vancomycin
- Vendor Tracking Identifier
- Venous Thromboembolism
- Venous Thromboembolism (VTE) Prophylaxis
- Ventilated
- Ventilator Day 1
- Ventilator Final Day
- Ventilator-Associated Pneumonia Rate
- Violence Risk to Others
- Violence Risk to Self
- Visible Assessment
- Vital Sign Monitoring
- Voluntary Turnover
- Warning Signs and Symptoms of Stroke
- Written Discharge Instructions
- deleted from ACHF - Care Transition Record-Condition or Functional Status at Discharge
- try
Risk Adjustment: Yes. Applied through direct standardization. This section has been moved to the ORYX Risk Adjustment Guide. This guide is available to the public on the Joint Commissions website and, in addition, it is available to performance measurement systems via the Joint Commissions extranet site for measurement systems (PET)
Data Elements
Data Collection Approach: Retrospective data sources for required data elements include administrative data and medical records.
Data Accuracy: Variation may exist in the assignment of ICD-9 codes; therefore, coding practices may require evaluation to ensure consistency.
Measure Analysis Suggestions: In order to identify areas for improvement, hospitals may want to review results based on specific ICD-9 codes or patient populations. Data could then be analyzed further determine specific patterns or trends to help reduce cesarean sections.
Sampling: Yes. For additional information see the Sampling Section.
Data Reported As: Aggregate rate generated from count data reported as a proportion.
Selected References:
- Agency for Healthcare Research and Quality. (2002). AHRQ Quality IndicatorsGuide to Inpatient Quality Indicators: Quality of Care in HospitalsVolume, Mortality, and Utilization. Revision 4 (December 22, 2004). AHRQ Pub. No. 02-RO204.
- Alfirevic, Z., Edwards, G., & Platt, M.J. (2004). The impact of delivery suite guidelines on intrapartum care in standard primigravida. Eur J Obstet Gynecol Reprod Biol.115:28-31.
- American College of Obstetricians and Gynecologists. (2000). Task Force on Cesarean Delivery Rates. Evaluation of Cesarean Delivery. (Developed under the direction of the Task Force on Cesarean Delivery Rates, Roger K. Freeman, MD, Chair, Arnold W. Cohen, MD, Richard Depp III, MD, Fredric D. Frigoletto Jr, MD, Gary D.V. Hankins, MD, Ellice Lieberman, MD, DrPH, M. Kathryn Menard, MD, David A. Nagey, MD, Carol W. Saffold, MD, Lisa Sams, RNC, MSN and ACOG Staff: Stanley Zinberg, MD, MS, Debra A. Hawks, MPH, and Elizabeth Steele).
- Bailit, J.L., Garrett, J.M., Miller, W.C., McMahon, M.J., & Cefalo, R.C. (2002). Hospital primary cesarean delivery rates and the risk of poor neonatal outcomes. Am J Obstet Gynecol. 187(3):721-7.
- Bailit, J. & Garrett, J. (2003). Comparison of risk-adjustment methodologies. Am J Obstet Gynecol.102:45-51.
- Bailit, J.L., Love, T.E., & Dawson, N.V. (2006). Quality of obstetric care and risk-adjusted primary cesarean delivery rates. Am J Obstet Gynecol.194:402.
- Bailit, J.L. (2007). Measuring the quality of inpatient obstetrical care. Ob Gyn Sur. 62:207-213.
- Berkowitz, G.S., Fiarman, G.S., Mojica, M.A., et al. (1989). Effect of physician characteristics on the cesarean birth rate. Am J Obstet Gynecol. 161:146-9.
- California Office of Statewide Hospital Planning and Development. (2006). Utilization Rates for Selected Medical Procedures in California Hospitals, Retrieved from the Internet on February 11, 2010 at: http://www.oshpd.ca.gov/HID/Products/PatDischargeData/ResearchReports/HospIPQualInd/Vol-Util_IndicatorsRpt/2007Util.pdf
- Cleary, R., Beard, R.W., Chapple, J., Coles, J., Griffin, M., & Joffe, M. (1996). The standard primipara as a basis for inter-unit comparisons of maternity care. Br J Obstet Gynecol. 103:223-9.
- Coonrod, D.V., Drachman, D., Hobson, P., & Manriquez, M. (2008). Nulliparous term singleton vertex cesarean delivery rates: institutional and individual level predictors. Am J Obstet Gynecol. 694-696.
- DiGiuseppe, D.L., Aron, D.C., Payne, S.M., Snow, R.J., Dieker, L., & Rosenthal, G.E. (2001). Risk adjusting cesarean delivery rates: a comparison of hospital profiles based on medical record and birth certificate data. Health Serv Res.36:959-77.
- Gould, J., Danielson, B., Korst, L., Phibbs, R., Chance, K.,& Main, E.K., et al. (2004). Cesarean delivery rate and neonatal morbidity in a low-risk population. Am J Obstet Gynecol, 104:11-19.
- Goyert, G.L., Bottoms, F.S., Treadwell, M.C., et al. (1989). The physician factor in cesarean birth rates. N Engl J Med.320:706-9.
- Le Ray, C., Carayol, M., Zeitlin, J., Berat, G., & Goffinet, F. (2006). Level of perinatal care of the maternity unit and rate of cesarean in low-risk nulliparas. Am J Obstet Gynecol. 107:1269-77.
- Luthy, D.A., Malmgren, J.A., Zingheim, R.W., & Leininger, C.J. (2003). Physician contribution to a cesarean delivery risk model. Am J Obstet Gynecol.188:1579-85.
- Main, E.K. (1999). Reducing cesarean birth rates with data-driven quality improvement activities. Peds. 103: 374-383.
- Main E.K., Bloomfield, L., & Hunt, G. (2004). Development of a large-scale obstetric quality-improvement program that focused on the nulliparous patient at term. Am J Obstet Gynecol.190:1747-58.
- Main, E.K., Moore, D., Farrell, B., Schimmel, L.D., Altman, R.J., Abrahams, C., et al., (2006). Is there a useful cesarean birth measure? Assessment of the nulliparous term singleton vertex cesarean birth rate as a tool for obstetric quality improvement. Am J Obstet Gynecol. 194:1644-51.
- Menacker, F. (2005).Trends in cesarean rates for first births and repeat cesarean rates for low-risk women: United States, 1990-2003. Nat Vital Stat Rep. 54(4): 1-5.
- Romano, P.S., Yasmeen, S., Schembri, M.E., Keyzer, J.M., & Gilbert, W.M. (2005). Coding of perineal lacerations and other complications of obstetric care in hospital discharge data. Am J Obstet Gynecol.106:717-25.
- U.S. Department of Health and Human Services. (2000). Healthy People 2010: Understanding and Improving Health. 2nd ed. Washington, DC: U.S. Government Printing Office. Measure 16-9.
- Yasmeen, S., Romano, P.S., Schembri, M.E., Keyzer, J.M., & Gilbert, W.M. (2006). Accuracy of obstetric diagnoses and procedures in hospital discharge data. Am J Obstet Gynecol. 194:992-1001.
Original Performance Measure Source / Developer:
California Maternal Quality Care Collaborative
Measure Algorithm:
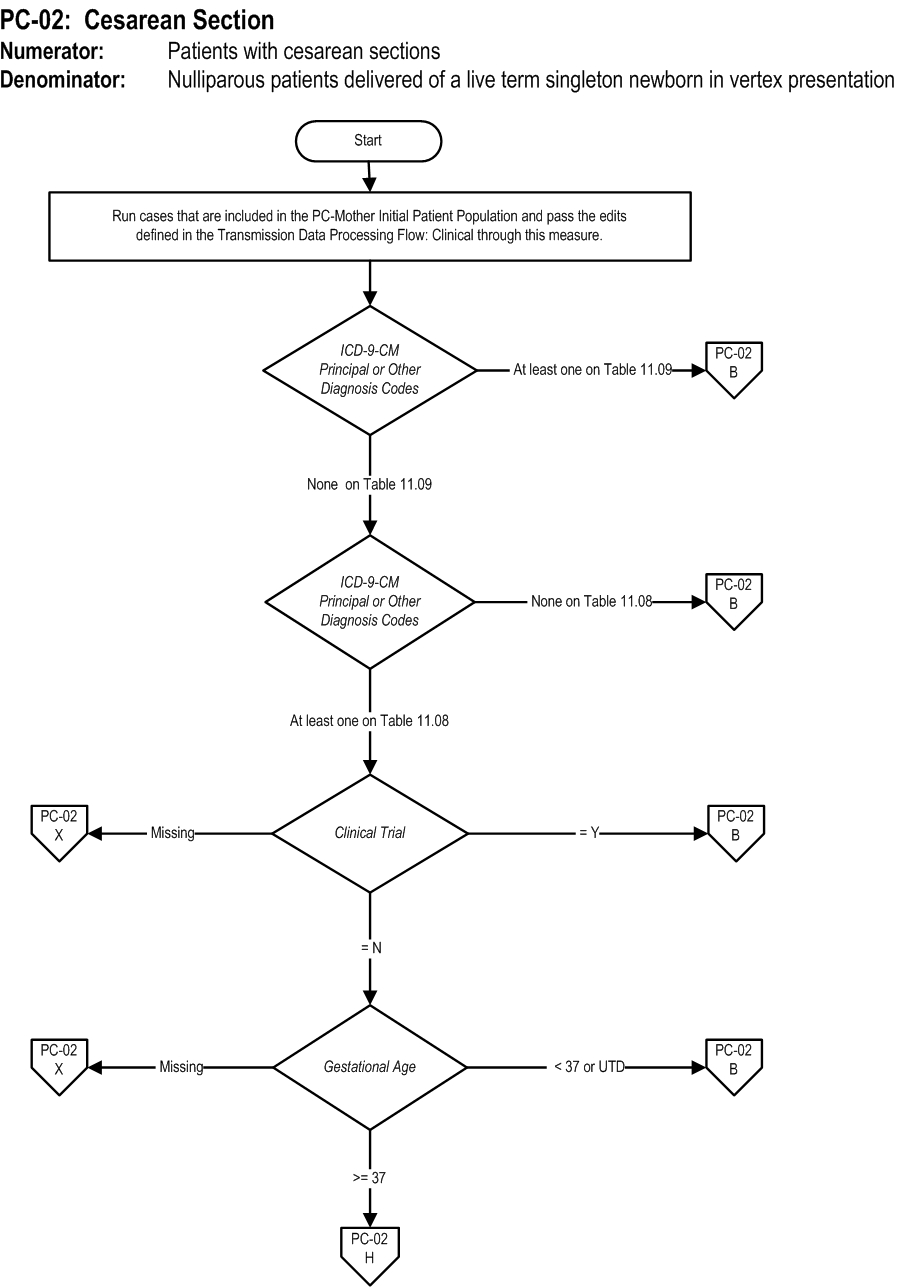

Measure Information Form PC-02
Specifications Manual for Joint Commission National Quality Measures (v2015A1)
01/01/2015 - 09/30/2015