Measure Information Form
Version 2022B2
Measure Information Form
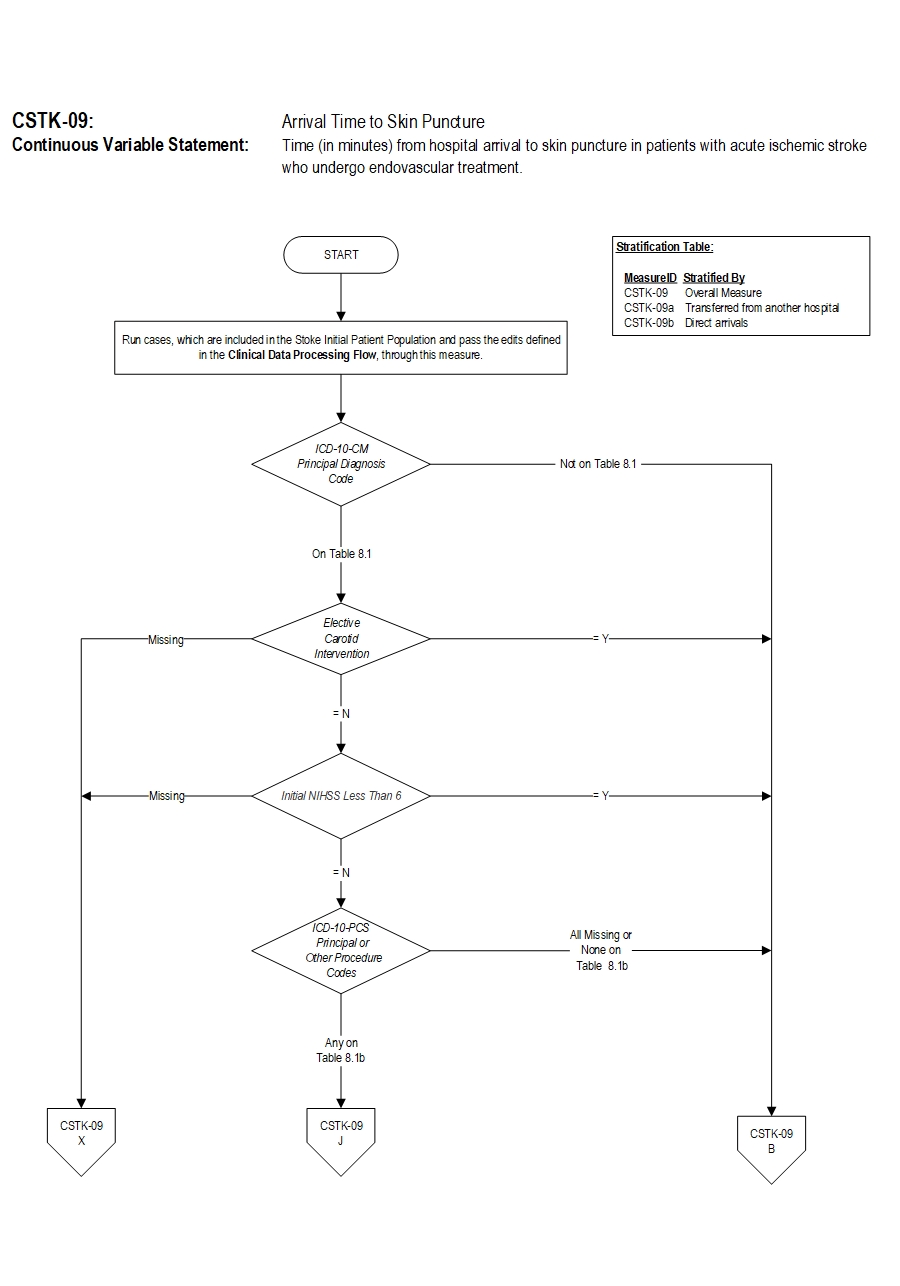
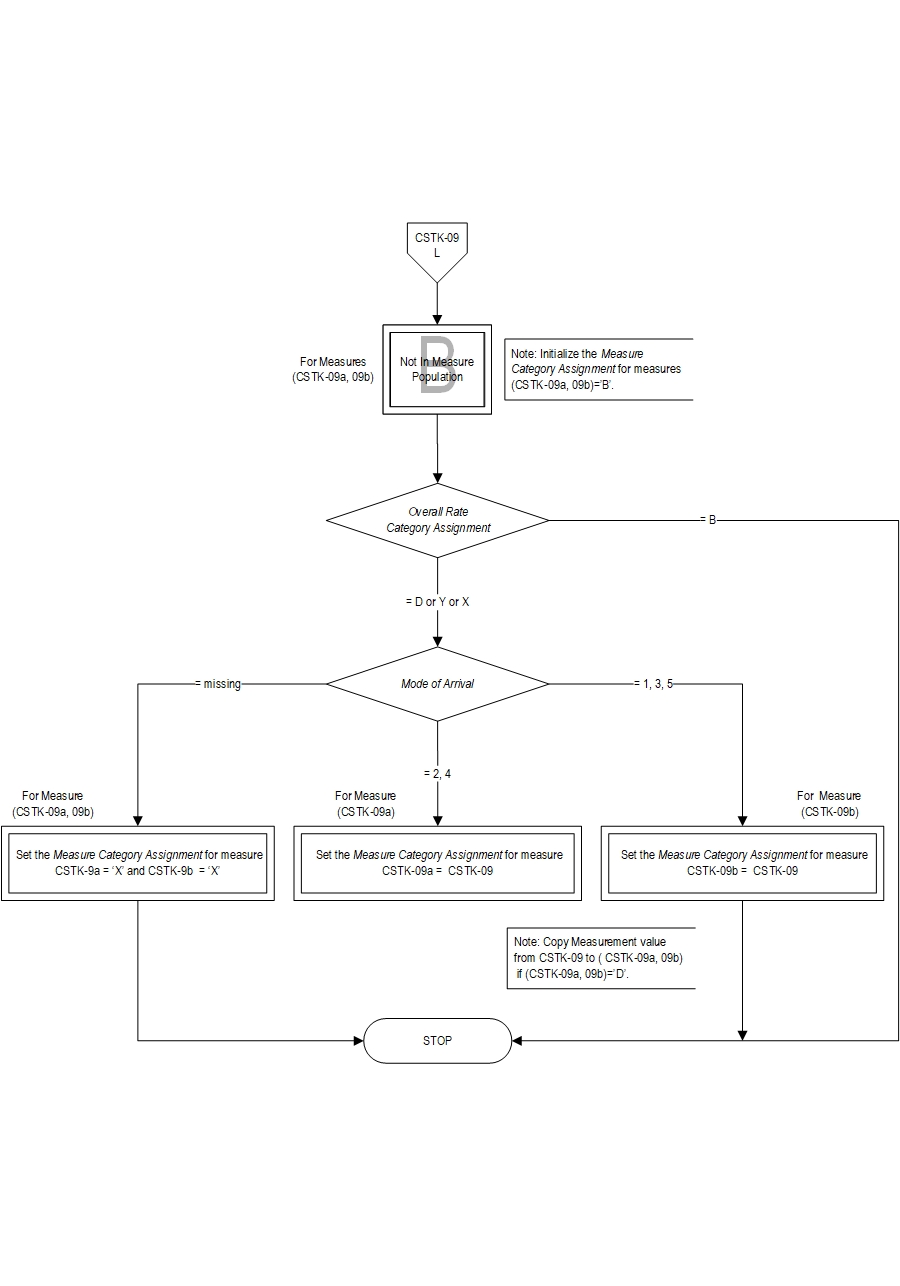
The CSTK-09 measure is reported as an overall rate (i.e., median time in minutes) which includes ischemic stroke patients who undergo EVT. CSTK-09a and CSTK-09b are subsets of the overall rate, and stratified by the mode of patient arrival to the hospital.
Rationale: Timely recanalization of an occluded intracerebral artery is a strong predictor of improved functional outcome and reduced mortality in patients with an acute ischemic stroke. Initiation of intra-venous (IV) alteplase within three hours of time last known well is recommended first before attempting other treatment; however, endovascular treatment (EVT) with mechanical retrieval devices is also recommended after IV thrombolysis failure or lapse of the therapeutic window. For eligible patients, initiation of EVT (e.g., groin puncture) within 6 hours of stroke symptom onset using a stent retriever is preferred (Powers WJ, et. al., 2015). Findings from clinical trials published in 2018 ( i.e., DAWN, DEFUSE 3) have reported the benefits of mechanical thrombectomy in the extended window up to 24 hours of last known well for select ischemic stroke patients meeting certain criteria. The use of mechanical thrombectomy devices other than stent retrievers as first-line devices for mechanical thrombectomy may be reasonable in some circumstances, but stent retrievers remain the first choice (Powers WJ, et. al., 2018).Since “time is brain”, the overall speed of the revascularization process is an important and appropriate measure. In multicenter clinical trials of intra-arterial catheter-directed therapies, the probability of good outcome as defined by a Modified Rankin Score of 0-2 at 90 days decreased as time to angiographic revascularization increased. It is estimated that for every 30-minute delay in time to revascularization, there is a 10% decrease in the likelihood of a good outcome from EVT. Five randomized clinical trials (RCTs) published in 2015 demonstrated the benefit of timely endovascular therapy in select patients with acute ischemic stroke due to large vessel occlusion (Jahan R et al., 2019).
American Heart Association Get With The Guidelines® (GWTG) sets a goal for Door-To-Puncture (DTP) Time within 90 minutes. Recent studies have reported that shorter DTP times may be achieved. Jahan and colleagues studied the time-benefit relationship in a large cohort of 6756 acute ischemic stroke patients from the GWTG clinical registry who underwent endovascular therapy within 8 hours of symptom onset. Findings from this study suggest that national quality target DTP times could be within 75 minutes for patients arriving directly to the hospital via emergency medical services (EMS) and within 45 minutes for patients transferred from another acute care hospital.
Type Of Measure: Process Improvement Noted As: Decrease in the median valueIncluded Populations:Excluded Populations:
- Discharges with ICD-10-CM Principal Diagnosis Code for ischemic stroke as defined in Appendix A, Table 8.1 for ICD-10 codes,
AND- Patients with documented Mechanical Endovascular Reperfusion Therapy (ICD-10-PCS Principal or Other Procedure Codes as defined in Appendix A, Table 8.1b for ICD-10 codes).
Data Elements:
- Patients less than 18 years of age
- Patients who have a Length of Stay > 120 days
- Patients admitted for Elective Carotid Intervention
- Patients who have an Initial NIHSS Less Than 6
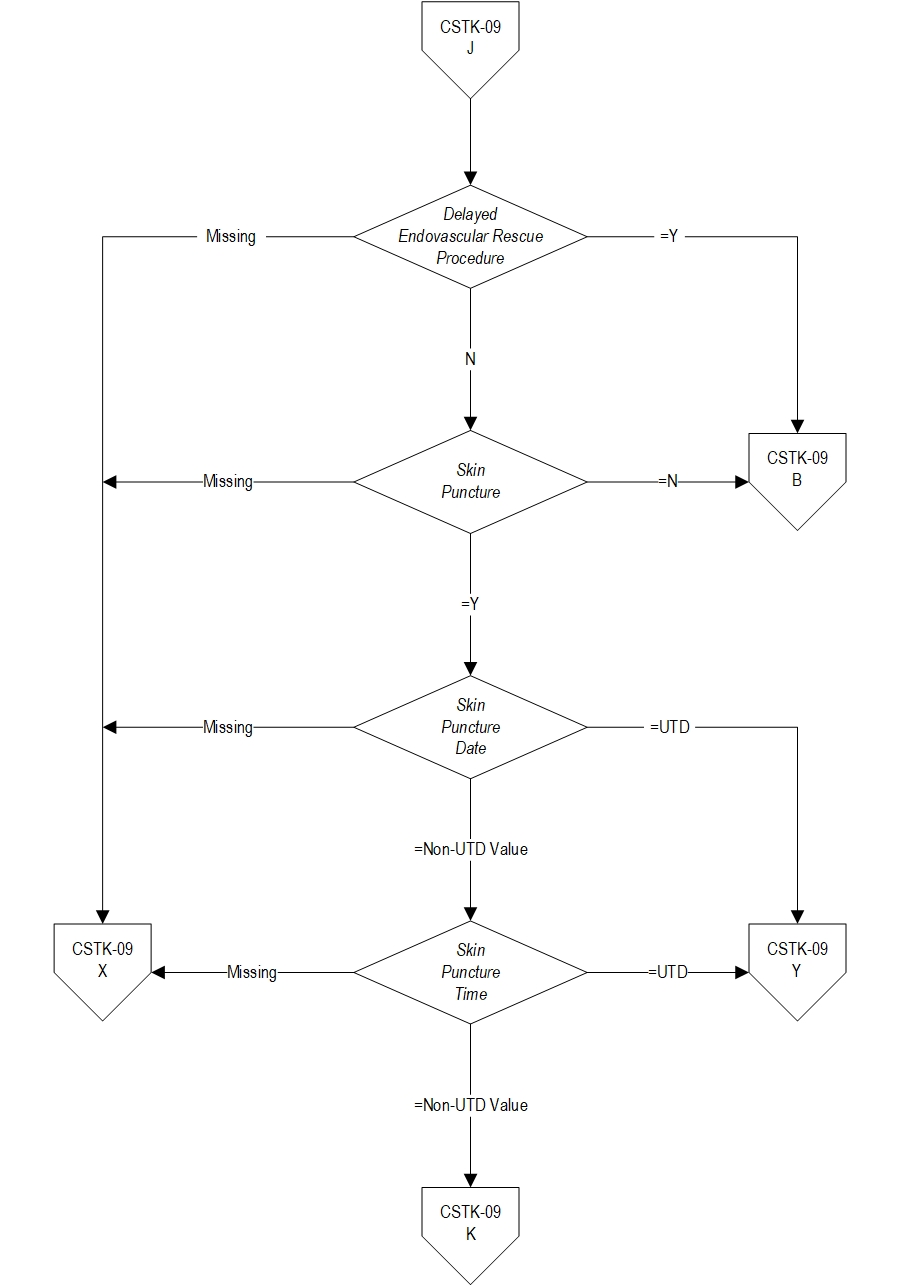
- Patients who have a Delayed Endovascular Rescue Procedure later than 8 hours after hospital arrival (ICD-10-PCS Principal or Other Procedure Codes as defined in Appendix A, Table 8.1a or Table 8.1b)
- Admission Date
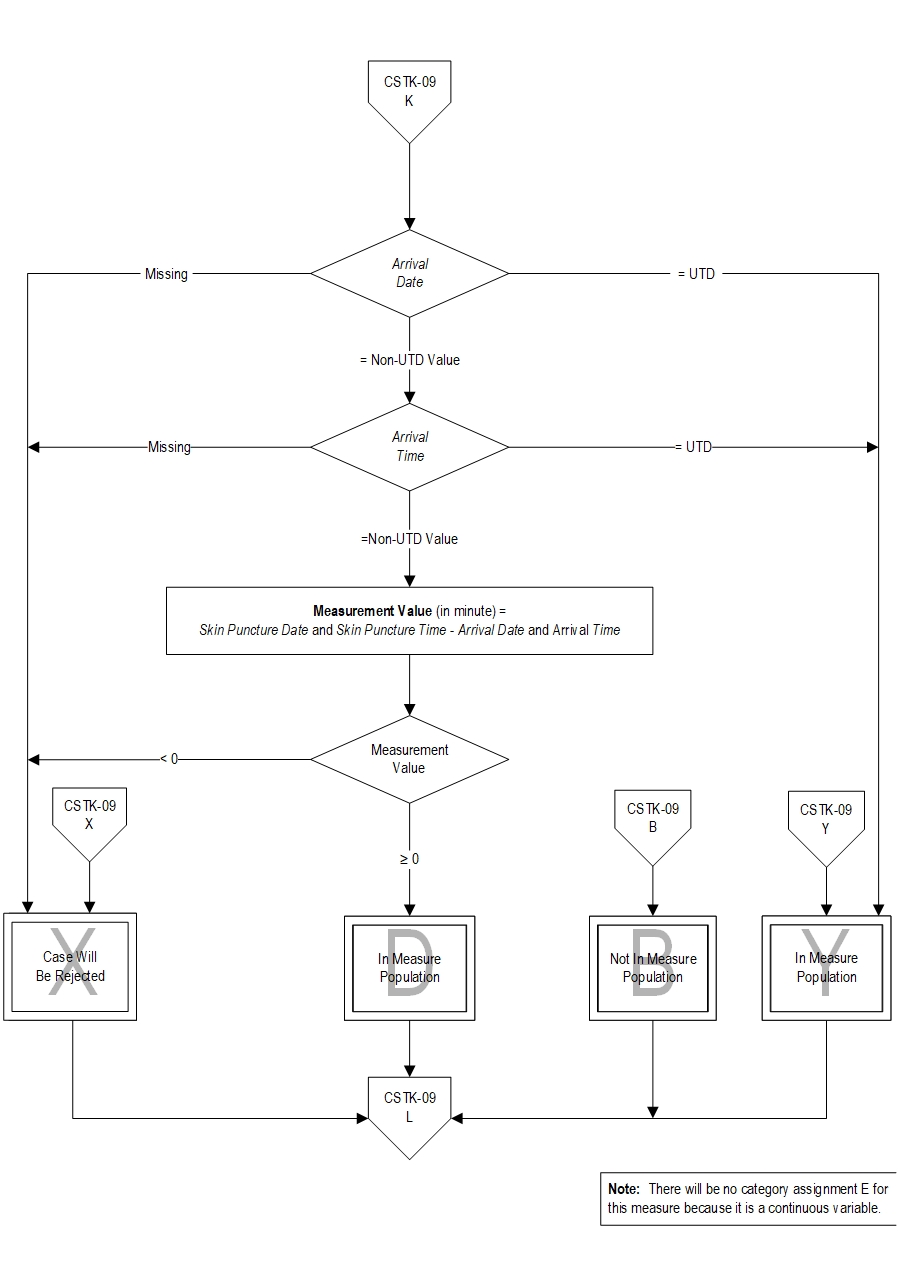
- Arrival Date
- Arrival Time
- Birthdate
- Delayed Endovascular Rescue Procedure
- Discharge Date
- Elective Carotid Intervention
- ICD-10-CM Principal Diagnosis Code
- ICD-10-PCS Other Procedure Codes
- ICD-10-PCS Other Procedure Dates
- ICD-10-PCS Principal Procedure Code
- ICD-10-PCS Principal Procedure Date
- Initial NIHSS Less Than 6
- Mode of Arrival
- Skin Puncture
- Skin Puncture Date
- Skin Puncture Time
- Adams HP, Brott TG, Furlan AJ, Gomez CR, Grotta J, Helgason CM, Kwiatkowski T, Lyden PD, Marler JR, Torner J, et. al. Guidelines for thrombolytic therapy for acute stroke: a supplement to the guidelines for the management of patients with acute ischemic stroke. Circulation. 1996;94:1167-1174.
- Albers GW, Marks MP, Kemp S, Christensen S, Tsai JP, Ortega-Gutierrez S, et. al. Thrombectomy for stroke at 6 to 16 hours with selection by perfusion imaging. NEJM. 2018;378(8): 708-718.
- Antman EM, Anbe DT, Armstrong PW, Bates ER, Green LA, Hand M, et al. ACC/AHA guidelines for the management of patients with ST-elevation myocardial infarction: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee to Revise the 1999 Guidelines for the Management of Patients With Acute Myocardial Infarction). 2004.
- Antman EM, Hand M, Armstrong PW, Bates ER, Green LA, Halasyamani LK, et al. 2007 focused update of the ACC/AHA 2004 Guidelines for the Management of Patients With ST-Elevation Myocardial Infarction: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Group to Review New Evidence and Update the ACC/AHA 2004 Guidelines for the Management of Patients With ST-Elevation Myocardial Infarction). J Am Coll Cardiol. 2008;51:210—-47.
- Campbell BCV, Mitchell PJ, Kleinig TJ, Dewey HM, Churilov L, Yassi N, et. al. Endovascular therapy for ischemic stroke with perfusion-imaging selection. NEJM. 2015 Mar;372(11): 1009-17.
- Demchuk AM, Goyal M, Monon BK, Eesa M, Ryckborst KJ, Kamal N, et. al. Endovascular treatment for Small Core and Anterior circulation Proximal occlusion with Emphasis on minimizing CT to recanalization times (ESCAPE) trial: methodology. Int J Stroke. 2015 Apr;10(3): 429-38.
- Furlan A, Higashida R, Wechsler L, et. al. Intra-arterial prourokinase for acute ischemic stroke. The PROACT II study; a randomized controlled trial. Prolyse in Actue Cerebral Thromboembolism. JAMA. 1999;282:2003-2011.
- Jahan R, Saver JL, Schwamm LH, Fonarow G, Liang L, Matsouaka RA, Xian Y, et al. Association Between Time to Treatment With Endovascular Reperfusion Therapy and Outcomes in Patients With Acute Ischemic Stroke Treated in Clinical Practice. JAMA. 2019;322(3):252-263.
- Jauch EC, Saver JL, Adams HP Jr, Bruno A, Connors JJ, Demaerschalk BM, Khatri P, et al. Guidelines for the early management of patients with acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2013;44:32-36.
- Khatari P, Abruzzo T, Yeatts SD, Nichols C, Broderick JP, Tomsick TA; IMS I and II Investigators. Good clinical outcome after ischemic stroke with successful revascularization is time-dependent. Neurology. 2009 Sep 29;73(13):1066-72.
- Khatari P, Hill MD, Palesch YY, et. al. Methodology of the Interventional Manaagement of Stroke III Trial. Int J Stroke. 2008;3:130-137.
- Leifer D, Bravata DM, Connors JJ III, Hinchey JA, Jauch EC, Johnston SC, Latchaw R, Likosky W, Ogilvy C, Qureshi AI, Summers D, Sung GY, Williams LS, Zorowitz R, on behalf of the American Heart Association Special Writing Group of the Stroke Council, Atherosclerotic Peripheral Vascular Disease Working Group and Council on Cardiovascular Surgery and Anesthesia, and Council on Cardiovascular Nursing. Metrics for measuring quality of care in comprehensive stroke centers: detailed follow-up to Brain Attack Coalition comprehensive stroke center recommendations: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2011;42; 857.
- Nogueira RG, Jadhav AP, Haussen DC, Bonafe A, Budzik RF, Bhuva P, et. al. Thrombectomy 6 to 24 hours after stroke with a mismatch between deficit and infarct. NEJM. 2018;378(1): 11-21.
- Penumbra Pivotal Stroke Trial Investigators. The penumbra pivotal stroke trial: safety and effectiveness of a new generation of mechanical devices for clot removal in intracranial large vessel occlusive disease. Stroke. 2009;40:2761-2768.
- Powers WJ, Derdeyn CP, Biller J, Coffey CS, Jauch EC, Johnston KC, Johnston SC, Khalessi AA, Kidwell CS, Meschia JF, Ovbiagele B, Yavagal DR, on behalf of the American Heart Association Stroke Council. 2015 AHA/ASA focused update of the 2013 guidelines for the early management of patients with acute ischemic stroke regarding endovascular treatment: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2015;46; 3021-3035.
- Powers WJ, Rabinstein AA, Ackerson T, Adeoye OM, Bambakidis NC, Becker K, Biller J, et al; on behalf of the American Heart Association Stroke Council. 2018 Guidelines for the Early Management of Patients with Acute Ischemic Stroke: A Guideline for Healthcare Professionals From the American Heart Association/American Stroke Association. Stroke. 2018 Jan;49:e26-e30.
- Powers WJ, Rabinstein AA, Ackerson T, Adeoye OM, Bambakidis NC, Becker K, Biller J, et al. Guidelines for the Early Management of Patients with Acute Ischemic Stroke: 2019 Update to the 2018 Guidelines for the Early Management of Acute Ischemic Stroke. A Guideline for Healthcare Professionals From the American Heart Association/American Stroke Association. Stroke. 2019 Dec;50(12):e344-e418.
- Rha JH, Saver JL. The impact of recanalization on ischemic stroke outcome: a meta-analysis. Stroke.
- Sacks D, Black CM, Cognard C, Connors JJ III, Frei D, Gupta R, Jovin TG, Kluck B, Meyers PM, Murphy KJ, Ramee S, Rϋfenacht DA, Stallmeyer MJB, Vorwerk D. Multisociety consensus quality improvement guidelines for intraarterial catheter-directed treatment of acute ischemic stroke from the American Society of Neuroradiology, Canadian Interventional Radiology Association, Cardiovascular and interventional Radiological Society of Europe, Society for Cardiovascular Angiography and Interventions, Society of Interventional Radiology, Society of NeuroInterventional Surgery, European Society of Minimally Invasive Neurological Therapy, and Society of Vascular and Interventional Neurology. J Vasc Interv Radiol. 2013;24:151-163.
- Saver JL, Goyal M, Bonafe A, Diener HC, Levy EI, Pereira VM, et. al. Stent-retriever thrombectomy after intravenous t-PA vs. t-PA alone in stroke. NEJM. 2015 Apr: 1-11.
- Sharma VK, Teoh HL, Wong LYH, Su J, Ong BKC, and Chan BLP. Recanalization therapies in acute ischemic stroke: pharmacological agents, devices, and combinations. Stroke Research and Treatment. 2010.
- Smith WS, Sung G, Saver J, et. al. Mechanical thrombectomy for acute ischemic stroke: final results of the Multi MERCI trial. Stroke. 2008;39:1205-1212.
- Tarr R, Hsu D, Kulcsar Z, et. al. The POST trial: initial post-market experience of the Penumbra system: revascularization of large vessel occlusion in acute ischemic stroke in the United States and Europe. _J Neurointerv Surg. 2010;2:341-344.
- Turk AS, Frei D, Fiorella D, Mocco J, Baxter B, Siddiqui A, et. al. ADAPT FAST study: a direct aspiration first pass technique for acute stroke thrombectomy. J Neurointerv Surg. 2014 May;694): 260-4.
CPT® only copyright 2022 American Medical Association. All rights reserved. CPT® is a registered trademark of the American Medical Association.
You, your employees and agents are authorized to use CPT® only as contained in The Joint Commission performance measures solely for your own personal use in directly participating in healthcare programs administered by The Joint Commission. You acknowledge that the American Medical Association (“AMA”) holds all copyright, trademark and other rights in CPT®.
Any use not authorized herein is prohibited, including by way of illustration and not by way of limitation, making copies of CPT® for resale and/or license, transferring copies of CPT® to any party not bound by this Agreement, creating any modified or derivative work of CPT®, or making any commercial use of CPT®. License to use CPT® for any use not authorized herein must be obtained through the American Medical Association, Intellectual Property Services, AMA Plaza, 330 North Wabash Avenue, Suite 39300, Chicago, Illinois 60611-5885. Applications are available at the American Medical Association Web site, www.ama- assn.org/go/cpt.
U.S. Government Rights This product includes CPT® which is commercial technical data, which was developed exclusively at private expense by the American Medical Association, 330 North Wabash Avenue, Chicago, Illinois 60611. The American Medical Association does not agree to license CPT® to the Federal Government based on the license in FAR 52.227-14 (Data Rights - General) and DFARS 252.227-7015 (Technical Data - Commercial Items) or any other license provision. The American Medical Association reserves all rights to approve any license with any Federal agency.
Disclaimer of Warranties and Liabilities. CPT® is provided “as is” without warranty of any kind, either expressed or implied, including but not limited to the implied warranties of merchantability and fitness for a particular purpose. Fee schedules, relative value units, conversion factors and/or related components are not assigned by the AMA, are not part of CPT®, and the (AMA is not recommending their use. The AMA does not directly or indirectly practice medicine or dispense medical services. The responsibility for the content of this product is with The Joint Commission, and no endorsement by the AMA is intended or implied. The AMA disclaims responsibility for any consequences or liability attributable to or related to any use, non-use, or interpretation of information contained or not contained in this product.
This Agreement will terminate upon notice if you violate its terms. The AMA is a third party beneficiary to this Agreement.
Should the foregoing terms and conditions be acceptable to you, please indicate your agreement and acceptance by clicking below on the button labeled “accept”.