Release Notes:
Measure Information Form
Version 2018B1
Measure Information Form
Version 2018B1
Measure Information Form
| Set Measure ID | Performance Measure Name |
|---|---|
| PC-06.0 | Unexpected Complications in Term Newborns - Overall Rate |
| PC-06.1 | Unexpected Complications in Term Newborns - Severe Rate |
| PC-06.2 | Unexpected Complications in Term Newborns - Moderate Rate |
Severe complications include neonatal death, transfer to another hospital for higher level of care, severe birth injuries such as intracranial hemorrhage or nerve injury, neurologic damage, severe respiratory and infectious complications such as sepsis.
Moderate complications include diagnoses or procedures that raise concern but at a lower level than the list for severe e.g. use of CPAP or bone fracture. Examples include less severe respiratory complications e.g. Transient Tachypnea of the Newborn, or infections with a longer length of stay not including sepsis, infants who have a prolonged length of stay of over 5 days.
Rationale: The most important childbirth outcome for families is bringing home a healthy baby. While there have been measures developed to assess clinical practices and outcomes in preterm infants, there is a lack of metrics that assess the health outcomes of term infants who represent over 90% of all births. This measure addresses this gap and gauges adverse outcomes resulting in severe or moderate morbidity in otherwise healthy term infants without preexisting conditions. This measure also uses length of stay (LOS) modifiers to guard against overcoding and undercoding of diagnoses. Importantly, this metric also serves as a balancing measure for other maternal measures such as NTSV Cesarean rates and early elective delivery rates. The purpose of a balancing measure is to guard against any unanticipated or unintended consequences of quality improvement activities for these measures.Type Of Measure: Outcome Improvement Noted As: Decrease in the rate
Numerator Statement: Newborns with severe complications and moderate complications.
California Maternal Quality Care Collaborative
Included Populations:Denominator Statement: Liveborn single term newborns 2500 gm or over in birth weight.
Severe Complications:Moderate Complications:
- Death
- Transfer to another acute care facility for higher level of care
- ICD-10-CM Principal Diagnosis Code, ICD-10-CM Other Diagnosis Codes, ICD-10-PCS Principal Procedure Code or ICD-10-PCS Other Procedure Codes for Severe Morbidities as defined in Appendix A, Tables:
- 11.36 Severe Birth Trauma
- 11.37 Severe Hypoxia/Asphyxia
- 11.38 Severe Shock and Resuscitation
- 11.39 Neonatal Severe Respiratory Complications
- 11.40 Neonatal Severe Infection
- 11.41 Neonatal Severe Neurological Complications
- 11.42 Severe Shock and Resuscitation Procedures
- 11.43 Neonatal Severe Respiratory Procedures
- 11.44 Neonatal Severe Neurological Procedures
- Patients with Length of Stay greater than 4 days AND an ICD-10-CM Principal Diagnosis Code or ICD-10-CM Other Diagnosis Codes for Sepsis as defined in Appendix A, Table 11.45 Neonatal Severe Septicemia
Excluded Populations: None Data Elements:
- ICD-10-CM Principal Diagnosis Code, ICD-10-CM Other Diagnosis Codes, ICD-10-PCS Principal Procedure Code or ICD-10-PCS Other Procedure Codes for moderate complications as defined in Appendix A, Tables:
- 11.46 Moderate Birth Trauma
- 11.47 Moderate Respiratory Complications
- 11.48 Moderate Respiratory Complications Procedures
- ICD-10-CM Principal Diagnosis Code for single liveborn newborn as defined in Appendix A, Table 11.20.2 Single Liveborn Newborn-Vaginal AND Length of Stay greater than 2 days
OR
ICD-10-CM Principal Diagnosis Code for single liveborn newborn as defined in Appendix A, Table 11.20.3 Single Liveborn Newborn-Cesarean AND Length of Stay greater than 4 days
AND ANY
ICD-10-CM Principal Diagnosis Code, ICD-10-CM Other Diagnosis Codes, ICD-10-PCS Principal Procedure Code or ICD-10-PCS Other Procedure Codes for moderate complications as defined in Appendix A, Tables:
- 11.49 Moderate Birth Trauma with LOS
- 11.50 Moderate Respiratory Complications with LOS
- 11.51 Moderate Neurological Complications with LOS Procedures
- 11.52 Moderate Respiratory Complications with LOS Procedures
- 11.53 Moderate Infection with LOS
- Patients with Length of Stay greater than 5 days and NO ICD-10-CM Principal Diagnosis Code, ICD-10-CM Other Diagnosis Codes, ICD-10-PCS Principal Procedure Code or ICD-10-PCS Other Procedure Codes for jaundice or social indications as defined in Appendix A, Tables:
- 11.33 Neonatal Jaundice
- 11.34 Phototherapy
- 11.35 Social Indications
Included Populations: Single liveborn newborns with ICD-10-CM Principal Diagnosis Code for single liveborn newborn as defined in Appendix A, Table Number 11.20.1: Single Liveborn Newborn Excluded Populations:Risk Adjustment: No. Data Collection Approach: Retrospective data sources for required data elements include administrative data and medical records. Data Accuracy: Variation may exist in the assignment of ICD-10 codes; therefore, coding practices may require evaluation to ensure consistency. Measure Analysis Suggestions: In order to identify areas for improvement, hospitals may want to review results based on specific ICD-10 codes or patient populations. Data could then be analyzed further to determine specific patterns or trends to help reduce unexpected newborn complications. Sampling: No. Data Reported As: Aggregate rate generated from count data reported as a rate per 1000 livebirths. Selected References:Data Elements:
- Patients who are not born in the hospital or are part of multiple gestation pregnancies, with no ICD-10-CM Principal Diagnosis Code for single liveborn newborn as defined in Appendix A, Table Number 11.20.1: Single Liveborn Newborn
- ICD-10-CM Principal Diagnosis Code or ICD-10-CM Other Diagnosis Codes for birth weight < 2500g as defined in Appendix A, Table 11.12, 11.13, 11.14, 11.15, 11.16, 11.20 OR Birth Weight < 2500g
- Patients who are not term or with < 37 weeks gestation completed
- Patients whose term status or gestational age is missing and birthweight < 3000 gm
- ICD-10-CM Principal Diagnosis Code or ICD-10-CM Other Diagnosis Codes for congenital malformations and genetic diseases as defined in Appendix A, Table 11.30 Congenital Malformations
- ICD-10-CM Principal Diagnosis Code or ICD-10-CM Other Diagnosis Codes for pre-existing fetal conditions as defined in Appendix A, Table 11.31 Fetal Conditions
- ICD-10-CM Principal Diagnosis Code or ICD-10-CM Other Diagnosis Codes for maternal drug use exposure in-utero as defined in Appendix A, Table 11.32 Maternal Drug Use
- Martin JA, Hamilton BE, Ventura SJ et al. Births: Final data for 2010. National vital statistics reports; vol 61 no1. Hyattsville, MD: National Center for health Statistics. 2012
- Russo, C. A (Thomson Reuters) and Andrews, R.M (AHRQ). Potentially Avoidable Injuries to mothers and Newborns During Childbirth, 2006. HCUP Statistical Brief # 74. June 2009. Agency for Healthcare Research and Quality. Rockville, MD. http://www.hcup-us.ahrq.gov/reports/statsbriefs/sb74.pdf.
- Gregory KD, Fridman M, Shah S et al. Global measures of quality and patient safety-related childbirth outcomes: should we monitor adverse or ideal rates? Am J Obstet Gynecol 2009;200:681.e1-681.e7.
- Profit J, Zupancic JA, Gould JB et al. Implementing pay-for-performance in the neonatal intensive care unit. Pediatrics 2007;119:975-82
- Operative Vaginal Delivery. Practice Bulletin No. 17. American College of Obstetricians and Gynecologists. Obstet Gynecol 2000;1-8
- Shoulder dystocia. ACOG Practice Bulletin No. 40. American College of Obstetrician and Gynecologists. Obstet Gynecol 2002;100:1045-50
- Centers for Disease Control and Prevention. Prevention of Perinatal Group B Streptococcal Disease. MMWR 2010;59 (No. RR 10): 1-36 http://www.cdc.gov/mmwr/pdf/rr/rr5910.pdf
- Wilmink FA, Hukkelhoven CW, Lunshof, S et al. Neonatal outcome following elective cesarean section beyond 37 weeks of gestation: a 7- year retrospective analysis of a national registry.2010 Am J Obstet Gynecol 2002:250.e1-8
- Tita AT, Landon MB, Spong CY et al. Timing of Elective Repeat Cesarean Delivery at Term and Neonatal Outcomes. N Engl J Med 2009;360(2):111-20
- Hansen AK, Wisborg K, Uldbjerg N. Risk of respiratory morbidity in term infants delivered by elective cesarean section: cohort study. BMJ 2008;336:85
- Spong CY. Defining “Term” pregnancy: Recommendations from the defining “term” pregnancy workgroup. JAMA. 2013 Jun 19;309(23):2445-6.
- Zhang X and Kramer MS. Variations in Mortality and Morbidity by Gestational Age among Infants Born at Term. J Pediatr 2009;154:358-62
- Fleischman AR, Oinuma M and Clark SL. Rethinking the Definition of “Term Pregnancy”. Obstet Gynecol 2010;116(1)136-139
- Clark SL, Miller DD, Belfort MA, et al. Neonatal and maternal outcomes associated with elective term delivery. Am J Obstet Gynecol 2009;200:156.e1-156.e4
- Reddy UM, Bettegowda VR, Dias T et al. Term Pregnancy: A period of Heterogeneous Risk for Infant Mortality. Obstet Gynecol 2011;117:1279-1287
- "Unexpected Complications in Term Newborns.” California Maternal Quality Care Collaborative (CMQCC), 2018, www.cmqcc.org/focus-areas/quality-metrics/unexpected-complications-term-newborns.
California Maternal Quality Care Collaborative
Measure Algorithm:
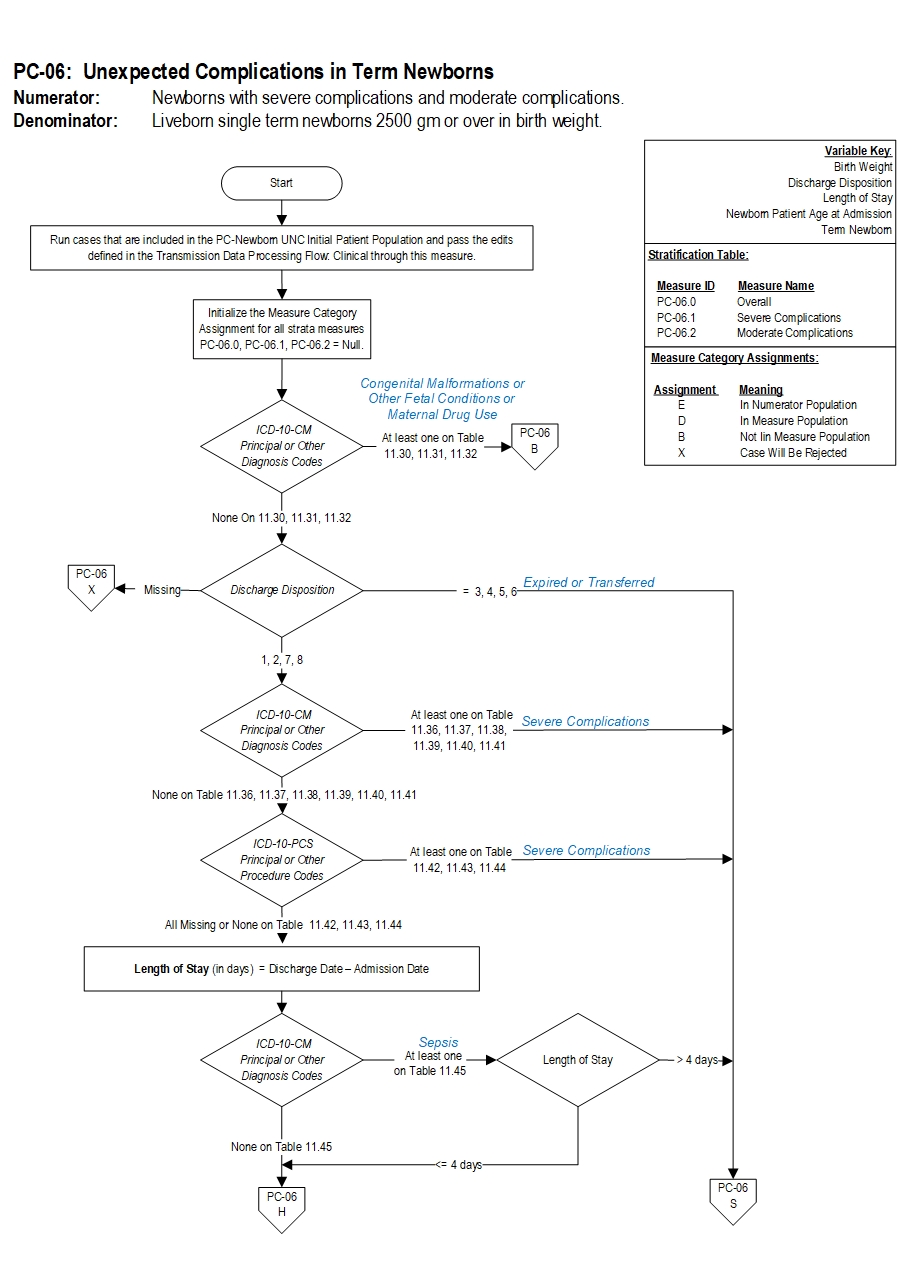
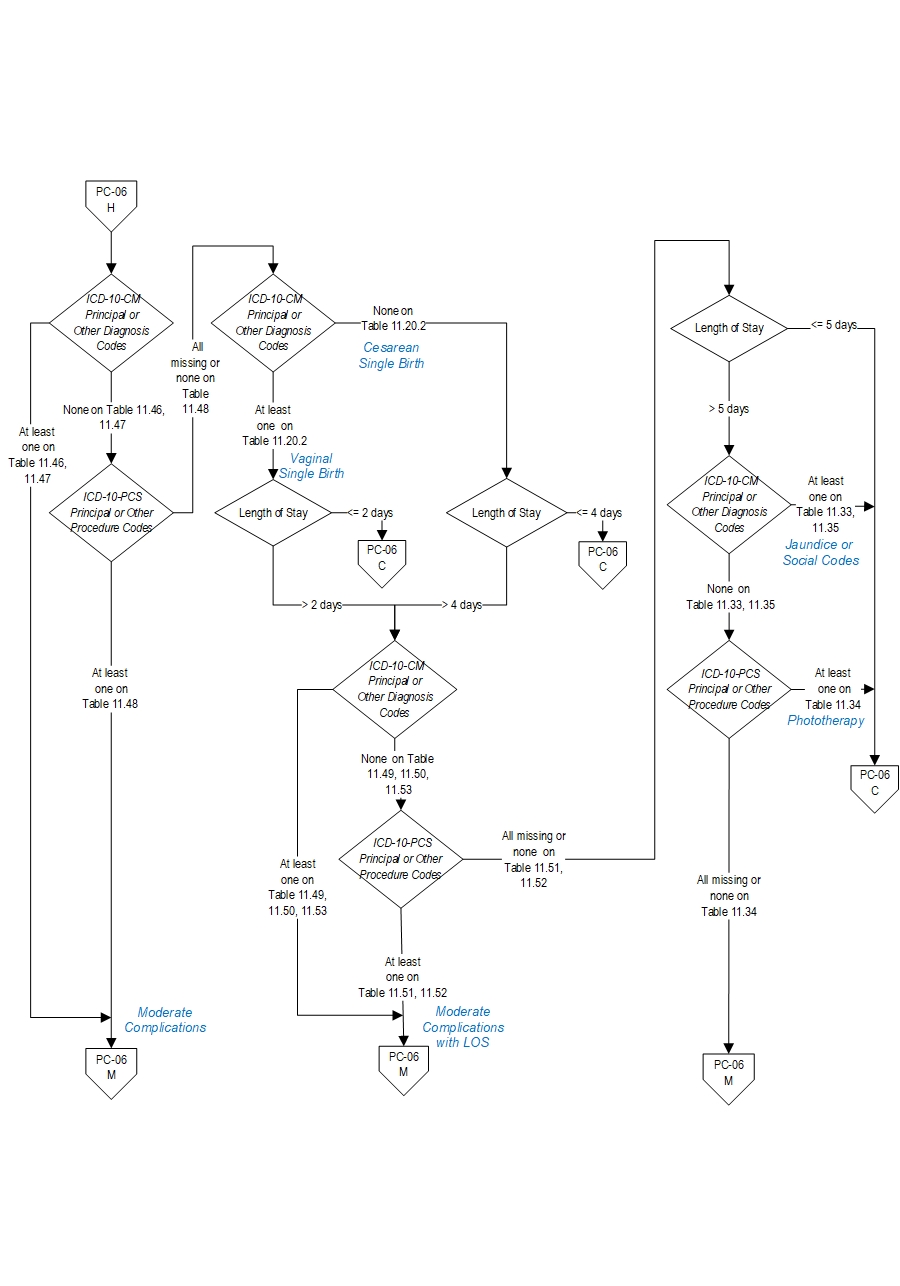
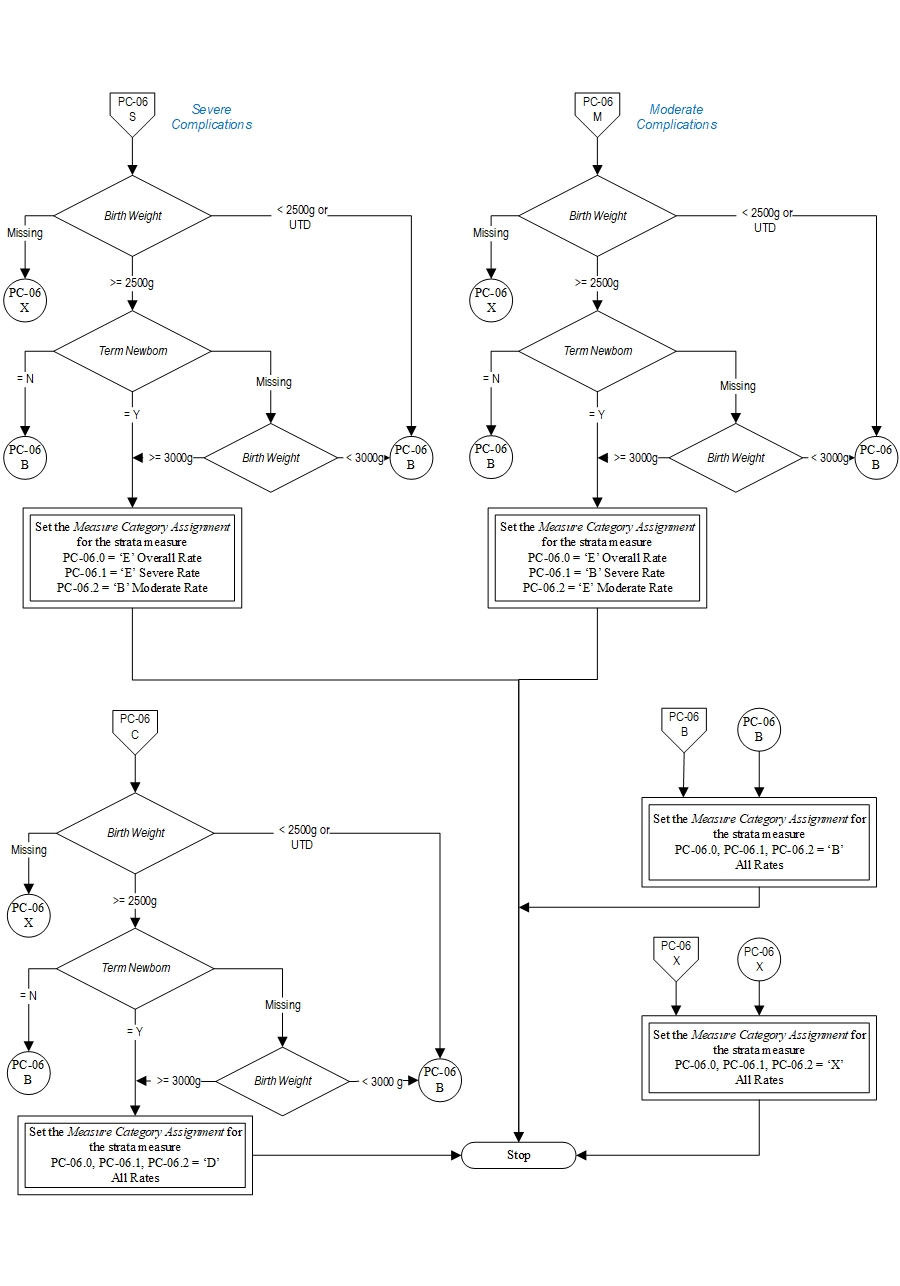



Questions? Ask Question to Joint Commission staff
Copyright © 2018 by The Joint Commission.