Release Notes:
Measure Information Form
Version 2018A1
Measure Information Form
Version 2018A1
**NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE**
Measure Information Form
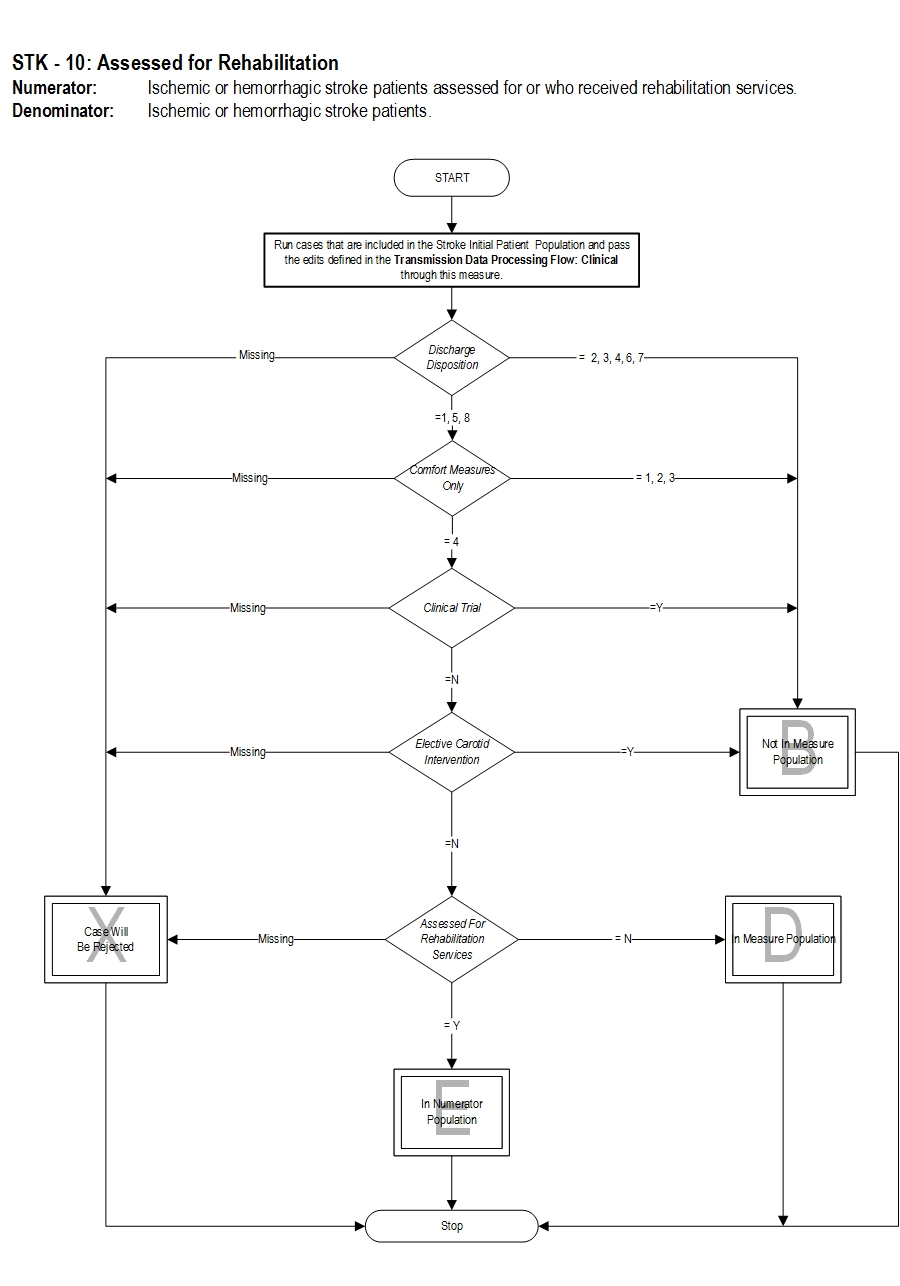
Numerator Statement: Ischemic or hemorrhagic stroke patients assessed for or who received rehabilitation services.
Risk Adjustment: No.
Data Collection Approach: Retrospective data sources for required data elements include administrative data and medical records. Some hospitals may prefer to gather data concurrently by identifying patients in the population of interest. This approach provides opportunities for improvement at the point of care/service. However, complete documentation includes the principal or other ICD-10 diagnosis and procedure codes, which require retrospective data entry.
Data Accuracy: Variation may exist in the assignment of ICD-10 codes; therefore, coding practices may require evaluation to ensure consistency.
Measure Analysis Suggestions: None
Sampling: Yes. Please refer to the measure set specific sampling requirements and for additional information see the Population and Sampling Specifications section.
Data Reported As: Aggregate rate generated from count data reported as a proportion.
Selected References: Included Populations: Not applicable Excluded Populations: None Data Elements:Denominator Statement: Ischemic or hemorrhagic stroke patients.
Included Populations: Discharges with an ICD-10-CM Principal Diagnosis Code for ischemic or hemorrhagic stroke as defined in Appendix A, Table 8.1 or Table 8.2. Excluded Populations:Data Elements:
- Patients less than 18 years of age
- Patients who have a Length of Stay greater than 120 days
- Patients with Comfort Measures Only documented
- Patients enrolled in clinical trials
- Patients admitted for Elective Carotid Intervention
- Patients discharged to another hospital
- Patients who left against medical advice
- Patients who expired
- Patients discharged to home for hospice care
- Patients discharged to a health care facility for hospice care
- Bates, B., J. Y. Choi, P. W. Duncan, J. J. Glasberg, G. D. Graham, R. C. Katz, K. Lamberty, et al. "Veterans Affairs/Department of Defense Clinical Practice Guideline for the Management of Adult Stroke Rehabilitation Care: Executive Summary." [In eng]. Stroke 36, no. 9 (Sep 2005): 2049-56.
- Centers for Disease Control and Prevention. "Prevalence and Most Common Causes of Disability among Adults--United States, 2005." [In eng]. MMWR Morb Mortal Wkly Rep 58, no. 16 (May 1 2009): 421-6.
- Duncan, P. W., R. Zorowitz, B. Bates, J. Y. Choi, J. J. Glasberg, G. D. Graham, R. C. Katz, K. Lamberty, and D. Reker. "Management of Adult Stroke Rehabilitation Care: A Clinical Practice Guideline." [In eng]. Stroke 36, no. 9 (Sep 2005): e100-43.
- Foley, N., R. Teasell, S. Bhogal, and M. Speechley. "The Efficacy of Stroke Rehabilitation." In, (2011): 1-50.
- http://www.ebrsr.com/evidence-review/5-efficacy-stroke-rehabilitation
- Gresham, G. E., P. W. Duncan, W. B. Stason, H. P. Adams, A. M. Adelman, D. N. Alexander, D. S. Bishop et al. "Post-stroke rehabilitation. Clinical practice guideline, no. 16. Rockville, MD: US Department of Health and Human Services." Public Health Service, Agency for Health Care Policy and Research (1995): 95-0062.
- Kalra, L., A. Evans, I. Perez, M. Knapp, C. Swift, and N. Donaldson. "A Randomised Controlled Comparison of Alternative Strategies in Stroke Care." [In eng]. Health Technol Assess 9, no. 18 (May 2005): iii-iv, 1-79.
- Keith, R. A. "Rehabilitation after Stroke: Cost-Effectiveness Analyses." [In eng]. J R Soc Med 89, no. 11 (Nov 1996): 631-3.
- Langhorne, P., B. O. Williams, W. Gilchrist, and K. Howie. "Do Stroke Units Save Lives?" [In eng]. Lancet 342, no. 8868 (Aug 14 1993): 395-8.
- "Management of Patients with Stroke: Rehabilitation, Prevention and Management of Complications, and Discharge Planning. A National Clinical Guideline." In, (2002). http://www.nhsggc.org.uk/content/mediaassets/pdf/HSD/sign64.pdf.
- Management of Stroke Rehabilitation Working Group. VA/DoD clinical practice guideline for the management of stroke rehabilitation. Washington (DC): Veterans Health Administration, Department of Defense; 2010.
- Moodie, M., D. Cadilhac, D. Pearce, C. Mihalopoulos, R. Carter, S. Davis, G. Donnan, and Scopes Study Group. "Economic Evaluation of Australian Stroke Services: A Prospective, Multicenter Study Comparing Dedicated Stroke Units with Other Care Modalities." [In eng]. Stroke 37, no. 11 (Nov 2006): 2790-5.
- Noorani, H. Z., B. Brady, L. McGahan, R. Teasell, B. Skidmore, and T. J. Doherty. "Stroke Rehabilitation Services: Systematic Reviews of the Clinical and Economic Evidence." In Ottawa: Canadian Coordinating, Office for Health Technology Assessment, 2003.
- Ottenbacher, K. J., and S. Jannell. "The Results of Clinical Trials in Stroke Rehabilitation Research." [In eng]. Arch Neurol 50, no. 1 (Jan 1993): 37-44.
- "Outcomes in Stroke Rehabilitation." Topics in Stroke Rehabilitation 12, no. 4 (Fall 2005): 1-10, 11-19, 20-27, 28-36, 37-49.
- "Rehabilitation Helps Stroke Patients Recover Skills ". American Academy of Physical Medicine and Rehabilitation, http://www.aapmr.org/patients/conditions/neurologic/Pages/recover.aspx.
- Saka, O., V. Serra, Y. Samyshkin, A. McGuire, and C. C. Wolfe. "Cost-Effectiveness of Stroke Unit Care Followed by Early Supported Discharge." [In eng]. Stroke 40, no. 1 (Jan 2009): 24-9.
- Stroke, National Institute of Neurological Disorders and. "Post-Stroke Rehabilitation Fact Sheet." http://www.ninds.nih.gov/disorders/stroke/poststrokerehab.htm.
- "Urgency Key but Perseverance Pays Off." American Academy of Physical Medicine and Rehabilitation. http://www.zoominfo.com/CachedPage/?archive_id=0&page_id=389260562&page_url=//www.aapmr.org/condtreat/rehab/strokeusa.htm&page_last_updated=2010-07-28T02:27:25&firstName=Charles&lastName=Levy
| Related Topics |
Questions? Ask Question to Joint Commission staff
Copyright © 2018 by The Joint Commission.