Release Notes:
Measure Information Form
Version 2016A1
**NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE**Measure Information Form
Measure Set: Perinatal Care(PC)
Set Measure ID: PC-01
Performance Measure Name: Elective Delivery
Description: Patients with elective vaginal deliveries or elective cesarean births at >= 37 and < 39 weeks of gestation completed
Rationale: For almost 3 decades, the American College of Obstetricians and Gynecologists (ACOG) and the American Academy of Pediatrics (AAP) have had in place a standard requiring 39 completed weeks gestation prior to ELECTIVE delivery, either vaginal or operative (ACOG, 1996). A survey conducted in 2007 of almost 20,000 births in HCA hospitals throughout the U.S. carried out in conjunction with the March of Dimes at the request of ACOG revealed that almost 1/3 of all babies delivered in the United States are electively delivered with 5% of all deliveries in the U.S. delivered in a manner violating ACOG/AAP guidelines. Most of these are for convenience, and result in significant short term neonatal morbidity (neonatal intensive care unit admission rates of 13- 21%) (Clark et al., 2009).
According to Glantz (2005), compared to spontaneous labor, elective inductions result in more cesarean births and longer maternal length of stay. The American Academy of Family Physicians (2000) also notes that elective induction doubles the cesarean delivery rate. Repeat elective cesarean births before 39 weeks gestation also result in higher rates of adverse respiratory outcomes, mechanical ventilation, sepsis and hypoglycemia for the newborns (Tita et al., 2009).
Type of Measure: Process
Improvement Noted As: Decrease in the rate
Numerator Statement: Patients with elective deliveries
Included Populations:
ICD-10-PCS Principal Procedure Code or ICD-10-PCS Other Procedure Codes for one or more of the following:
- Medical induction of labor as defined in Appendix A, Table 11.05 while not in Labor prior to the procedure
- Cesarean birth as defined in Appendix A, Table 11.06 and all of the following:
- not in Labor
- no history of a Prior Uterine Surgery
Excluded Populations: None
Data Elements:
Denominator Statement: Patients delivering newborns with >= 37 and < 39 weeks of gestation completed
Included Populations:
- ICD-10-PCS Principal Procedure Code or ICD-10-PCS Other Procedure Codes for delivery as defined in Appendix A, Table 11.01.1
- ICD-10-CM Principal Diagnosis Code or ICD-10-CM Other Diagnosis Codes for planned cesarean birth in labor as defined in Appendix A, Table 11.06.1
Excluded Populations:
- ICD-10-CM Principal Diagnosis Code or ICD-10-CM Other Diagnosis Codes for conditions possibly justifying elective delivery prior to 39 weeks gestation as defined in Appendix A, Table 11.07
- Less than 8 years of age
- Greater than or equal to 65 years of age
- Length of stay > 120 days
- Gestational Age < 37 or >= 39 weeks or UTD
Data Elements:
Risk Adjustment: No.
Data Collection Approach: Retrospective data sources for required data elements include administrative data and medical records.
Data Accuracy: Variation may exist in the assignment of ICD-10 codes; therefore, coding practices may require evaluation to ensure consistency.
Measure Analysis Suggestions: In order to identify areas for improvement, hospitals may want to review results based on specific ICD-10 codes or patient populations. Data could be analyzed further to determine specific patterns or trends to help reduce elective deliveries.
Sampling: Yes. For additional information see the Sampling Section.
Data Reported As: Aggregate rate generated from count data reported as a proportion.
Selected References:
- American Academy of Family Physicians. (2000). Tips from Other Journals: Elective induction doubles cesarean delivery rate, 61, 4.Retrieved December 29, 2008 at: http://www.aafp.org/afp/20000215/tips/39.html.
- American College of Obstetricians and Gynecologists. (November 1996). ACOG Educational Bulletin.
- Clark, S., Miller, D., Belfort, M., Dildy, G., Frye, D., & Meyers, J. (2009). Neonatal and maternal outcomes associated with elective delivery. [Electronic Version]. Am J Obstet Gynecol. 200:156.e1-156.e4.
- Glantz, J. (Apr.2005). Elective induction vs. spontaneous labor associations and outcomes. [Electronic Version]. J Reprod Med. 50(4):235-40.
- Tita, A., Landon, M., Spong, C., Lai, Y., Leveno, K., Varner, M, et al. (2009). Timing of elective repeat cesarean delivery at term and neonatal outcomes. [Electronic Version]. NEJM. 360:2, 111-120.
Original Performance Measure Source / Developer:
Hospital Corporation of America-Women's and Children's Clinical Services
Adopted for CMS Hospital Inpatient Quality Reporting Program FY 2015 and Stage 2 Medicare and Medicaid EHR Incentive Program
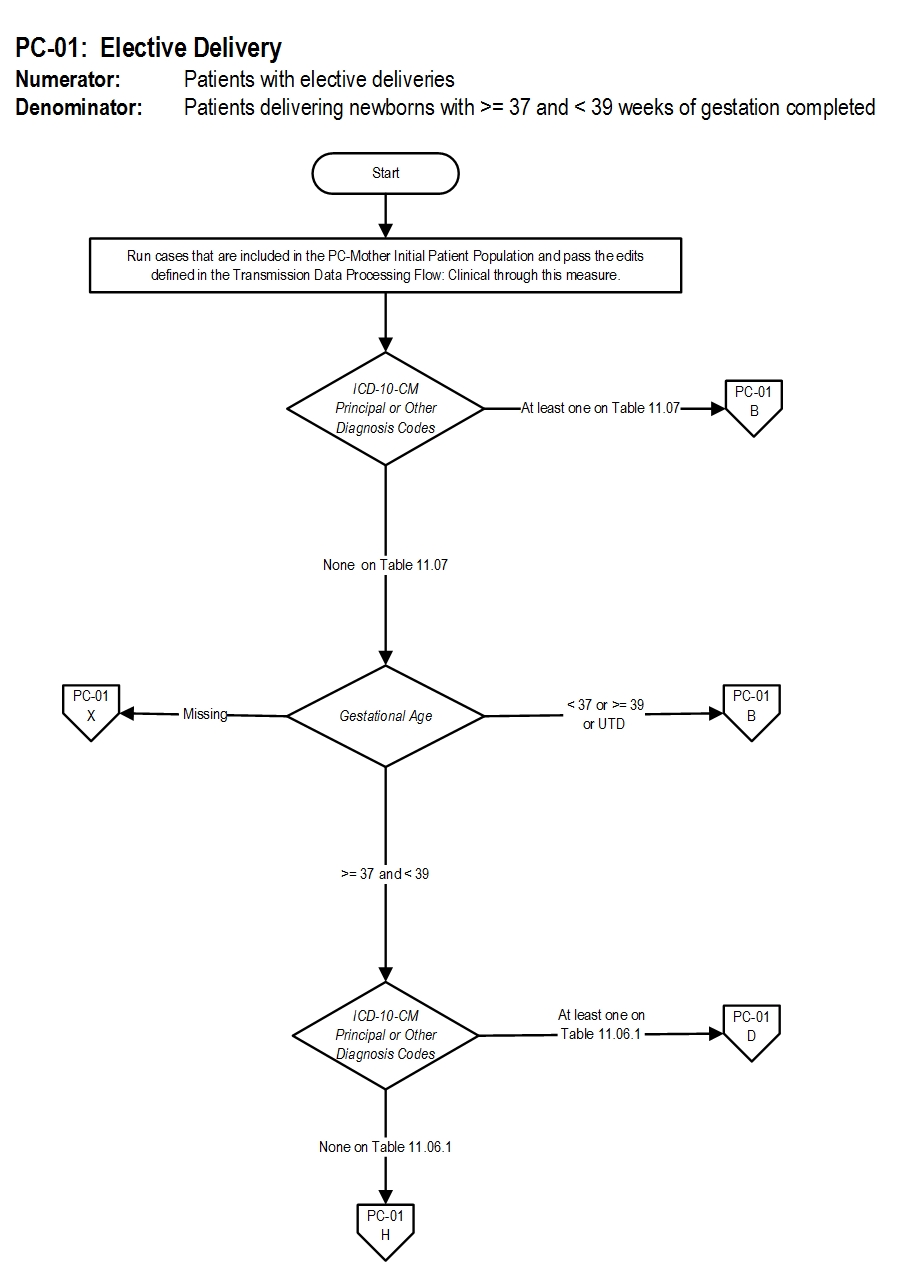
Measure Algorithm: